Spotting, in the context of menstruation, refers to light vaginal bleeding that occurs between regular periods. It is often described as a few drops or streaks of blood, lighter than a typical menstrual flow. While it can be alarming for some, spotting is a relatively common occurrence and can have a variety of causes, ranging from benign to more serious conditions. Understanding the nuances of spotting can empower individuals to better monitor their reproductive health and seek appropriate medical attention when necessary. This article will delve into the various facets of spotting on a period, exploring its potential causes, associated symptoms, and when it warrants a visit to a healthcare professional.
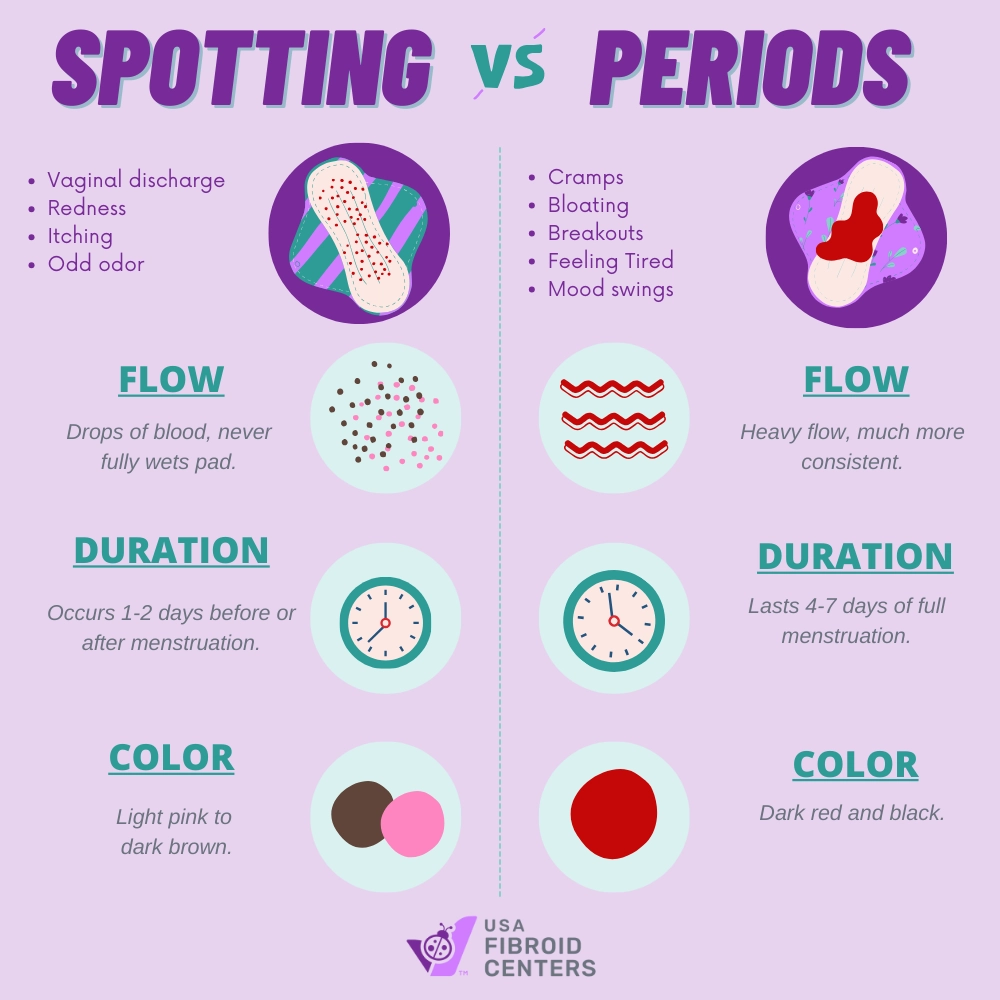
Understanding the Menstrual Cycle and Spotting
The menstrual cycle is a complex interplay of hormones that prepares the female reproductive system for potential pregnancy. A typical cycle lasts around 28 days, though variations are common. It begins with menstruation, the shedding of the uterine lining, which results in menstrual bleeding. Following menstruation, the ovaries release an egg (ovulation), and the uterine lining thickens in preparation for implantation. If fertilization does not occur, hormone levels drop, triggering the shedding of the uterine lining and the start of the next period. Spotting can occur at various points within this cycle, disrupting the expected flow of events.
Hormonal Fluctuations and Spotting
Hormonal fluctuations are a primary driver behind many instances of spotting. The delicate balance of estrogen and progesterone is crucial for maintaining a regular menstrual cycle. Any disruption to this balance can lead to irregular bleeding.
Mid-Cycle Ovulation Spotting
Ovulation, the release of an egg from the ovary, typically occurs around day 14 of a 28-day cycle. During ovulation, a small amount of bleeding can occur as the follicle ruptures to release the egg. This is known as ovulation spotting and is generally light, pinkish or brownish, and lasts for a day or two. It is often accompanied by other ovulation symptoms like changes in cervical mucus and mild pelvic discomfort. This type of spotting is considered normal and not a cause for concern.
Hormonal Birth Control and Spotting
Hormonal contraceptives, such as birth control pills, patches, rings, and injections, work by altering the body’s natural hormone levels to prevent pregnancy. These methods can lead to spotting, particularly during the initial months of use as the body adjusts to the artificial hormone levels. This is often referred to as “breakthrough bleeding.” For individuals using continuous or extended-cycle birth control, spotting can occur during hormone-free intervals or even while taking active pills. While usually harmless, persistent spotting while on hormonal birth control may indicate an issue with the chosen method or dosage, and consultation with a healthcare provider is recommended.
Perimenopause and Spotting
Perimenopause is the transitional period leading up to menopause, typically occurring in the late 40s and early 50s. During this time, hormonal levels, particularly estrogen and progesterone, become erratic, leading to irregular menstrual cycles. This irregularity often manifests as spotting between periods, lighter or heavier periods than usual, or skipped periods altogether. Spotting during perimenopause is a common symptom as the ovaries’ egg production declines and hormone production fluctuates. While generally a natural part of aging, it’s important for individuals to discuss any significant changes in their bleeding patterns with their doctor to rule out other potential causes.
Non-Hormonal Causes of Spotting
Beyond hormonal influences, several other factors can contribute to spotting between periods. These can range from simple lifestyle changes to underlying medical conditions.
Early Pregnancy and Implantation Bleeding
For sexually active individuals who could be pregnant, spotting can be an early sign of pregnancy. Implantation bleeding occurs when a fertilized egg attaches to the uterine wall, typically about 6 to 12 days after conception. This bleeding is usually very light, often just a few streaks of blood, and can be mistaken for a very light period. It may be pink, red, or brownish and can last from a few hours to a couple of days. It’s crucial to distinguish implantation bleeding from a menstrual period, as it signifies the beginning of a pregnancy. A pregnancy test can confirm or rule out pregnancy if spotting occurs around the expected time of a period.
Uterine Fibroids and Polyps

Uterine fibroids are non-cancerous growths that develop in the uterus, while polyps are small, benign growths that can occur in the uterine lining. Both fibroids and polyps can cause abnormal uterine bleeding, including spotting between periods. The location and size of these growths can influence the pattern of bleeding. Spotting caused by fibroids or polyps may be accompanied by other symptoms such as pelvic pain, pressure, or unusually heavy menstrual bleeding. Diagnosis often involves pelvic exams, ultrasounds, and sometimes hysteroscopy. Treatment depends on the size, location, and symptoms associated with the growths.
Infections and Inflammation
Various infections and inflammatory conditions affecting the reproductive organs can lead to spotting.
Cervicitis and Vaginitis
Cervicitis is inflammation of the cervix, often caused by sexually transmitted infections (STIs) like chlamydia or gonorrhea, or by non-infectious causes like allergic reactions to douches or spermicides. Vaginitis, inflammation of the vagina, can be caused by yeast infections, bacterial vaginosis, or trichomoniasis. Both cervicitis and vaginitis can irritate the cervical and vaginal tissues, leading to bleeding, especially after intercourse or during physical activity. This bleeding often appears as spotting and may be accompanied by discharge, itching, or pain. Prompt diagnosis and treatment of these infections are essential to prevent complications.
Pelvic Inflammatory Disease (PID)
Pelvic Inflammatory Disease (PID) is an infection of the reproductive organs that can affect the uterus, fallopian tubes, and ovaries. It is often a complication of untreated STIs. PID can cause a range of symptoms, including abnormal vaginal bleeding, such as spotting between periods. Other symptoms may include pelvic pain, fever, and painful intercourse. PID requires immediate medical attention and antibiotic treatment to prevent long-term damage to the reproductive system and infertility.
When to Seek Medical Advice for Spotting
While many instances of spotting are harmless, it’s essential to recognize when it might signal a more serious underlying issue. Consulting a healthcare professional is crucial for accurate diagnosis and appropriate management.
Persistent or Heavy Spotting
If spotting becomes persistent, meaning it occurs frequently or lasts for extended periods, it warrants medical evaluation. Similarly, if the spotting is heavier than just a few drops, resembling a light period that doesn’t progress to a full flow, it should be investigated. Persistent or heavy spotting could indicate conditions like uterine fibroids, polyps, hormonal imbalances not related to the normal cycle, or even early signs of miscarriage if pregnancy is a possibility. A doctor can perform examinations and tests to determine the cause.
Spotting Accompanied by Other Symptoms
The presence of other symptoms alongside spotting can be a red flag. These can include:
- Pelvic Pain or Cramping: While ovulation can cause mild discomfort, persistent or severe pelvic pain associated with spotting could indicate conditions like endometriosis, ovarian cysts, or pelvic inflammatory disease.
- Unusual Vaginal Discharge: Changes in the color, odor, or consistency of vaginal discharge, especially if accompanied by spotting, can point towards an infection.
- Pain During Intercourse (Dyspareunia): This can be a symptom of various conditions, including infections, inflammation, or structural abnormalities in the reproductive tract.
- Fever or Chills: These are signs of infection and require immediate medical attention, especially if accompanied by spotting or pelvic pain.
- Dizziness or Fainting: Significant blood loss, even if appearing as spotting, can lead to these symptoms and should be evaluated by a medical professional.

Post-Menopausal Spotting
Any bleeding or spotting that occurs after menopause, defined as 12 consecutive months without a menstrual period, is considered abnormal and requires immediate medical attention. Post-menopausal bleeding can be a symptom of more serious conditions, including endometrial polyps, uterine fibroids, or even endometrial cancer. Early detection and diagnosis are critical for effective treatment of these conditions.
In conclusion, spotting on a period, while often benign and attributed to hormonal fluctuations or normal physiological events, can also be an indicator of underlying medical concerns. By understanding the potential causes and recognizing when to seek professional advice, individuals can take proactive steps in managing their reproductive health and ensuring their well-being. Open communication with a healthcare provider is paramount in navigating the complexities of abnormal uterine bleeding and achieving peace of mind.
