Inflammatory Bowel Diseases (IBD), primarily Crohn’s disease and ulcerative colitis, represent chronic conditions that significantly impact the lives of millions worldwide. While historically understood through traditional medical research and clinical observation, the advent and rapid evolution of technology are revolutionizing our comprehension, diagnosis, management, and even the potential for future treatments of these complex gastrointestinal disorders. This article delves into the nature of Crohn’s disease and ulcerative colitis, exploring how technological innovation is shaping our understanding and approach to these challenging conditions.
The Biological Landscape of Inflammatory Bowel Diseases
At their core, Crohn’s disease and ulcerative colitis are characterized by inflammation within the digestive tract. However, the specific location, pattern, and depth of this inflammation differentiate them significantly. Understanding these fundamental biological differences is crucial for accurate diagnosis and effective treatment. Technological advancements are providing unprecedented insights into these intricate biological processes, moving beyond macroscopic observations to a molecular and genetic level.
Understanding Crohn’s Disease: A Transmural and Patchy Inflammation
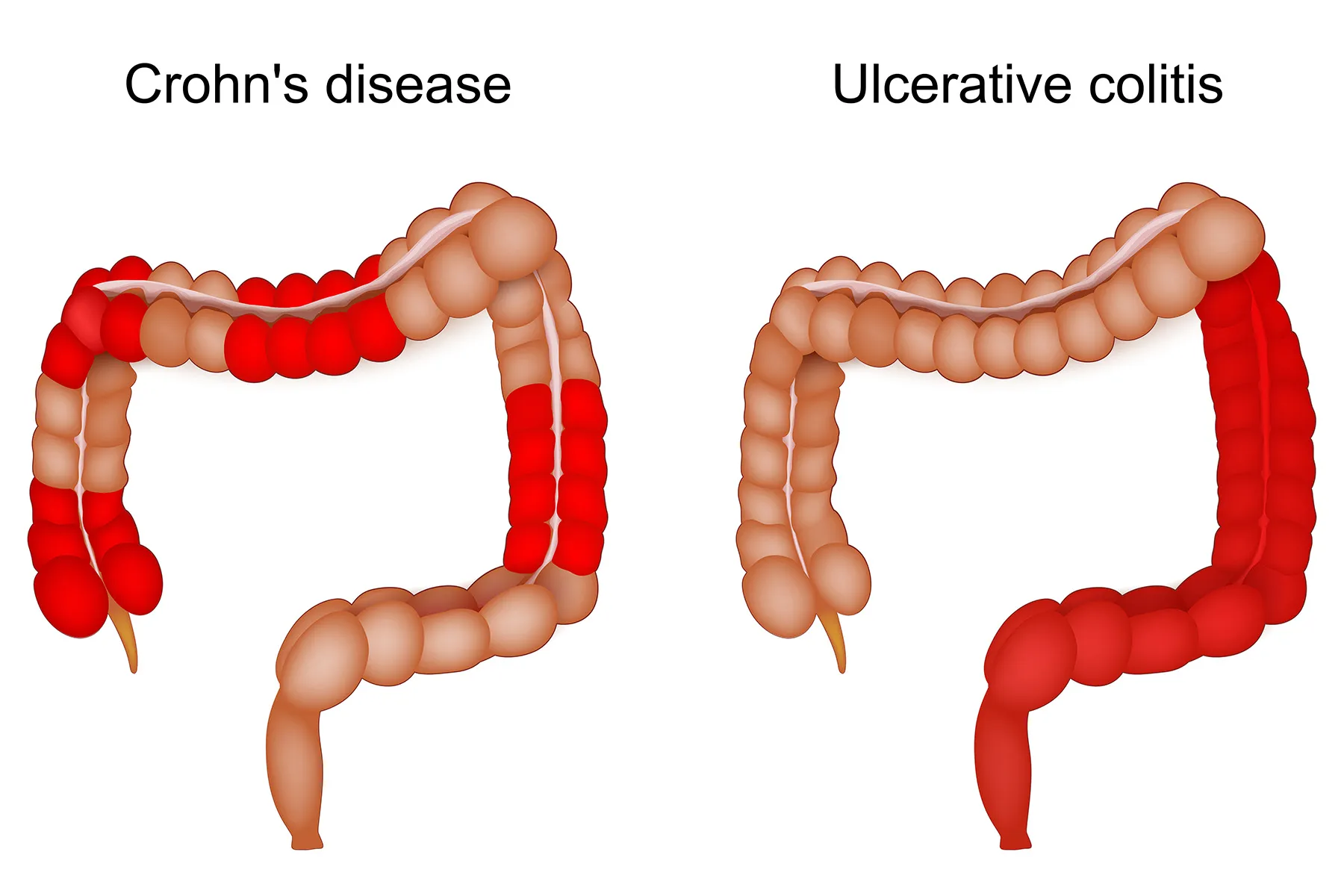
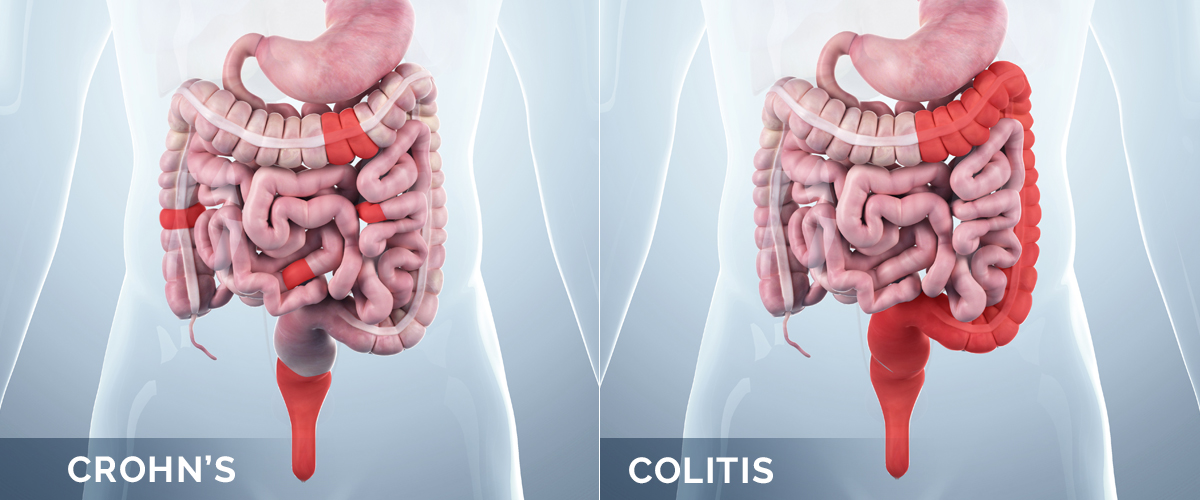
Crohn’s disease is a chronic inflammatory condition that can affect any part of the gastrointestinal tract, from the mouth to the anus. A hallmark of Crohn’s is its ability to affect all layers of the intestinal wall (transmural inflammation) and its tendency to occur in patches, with healthy tissue interspersed between inflamed areas. This characteristic “skip lesion” pattern can lead to complications such as strictures (narrowing of the intestine), fistulas (abnormal tunnels), and abscesses. The etiology of Crohn’s is complex, involving a dysregulated immune response in genetically susceptible individuals exposed to environmental triggers.
Technological Insights into Crohn’s Pathology:
- Advanced Imaging Modalities: While traditional endoscopy remains vital, technologies like Magnetic Resonance Enterography (MRE) and Computed Tomography Enterography (CTE) offer non-invasive, detailed visualization of the small intestine and colon. These techniques utilize sophisticated imaging algorithms and contrast agents to highlight inflammatory changes, transmural involvement, and complications like strictures and fistulas with remarkable precision. AI-powered image analysis is beginning to augment these modalities, identifying subtle patterns indicative of inflammation that might be missed by the human eye.
- Genomic and Proteomic Research: Large-scale genetic studies, such as genome-wide association studies (GWAS), have identified numerous genetic loci associated with an increased risk of Crohn’s disease. High-throughput sequencing technologies allow researchers to analyze the entire genome of patients, pinpointing specific gene variations that influence immune responses and gut barrier function. Proteomics, the study of proteins, is revealing the complex molecular pathways involved in inflammation, identifying potential therapeutic targets.
- Microbiome Analysis: The gut microbiome, the vast community of microorganisms residing in the digestive tract, plays a critical role in immune homeostasis. Advanced sequencing technologies (e.g., 16S rRNA sequencing, shotgun metagenomics) are being used to profile the microbial composition of patients with Crohn’s disease. Disruptions in the microbiome, known as dysbiosis, are increasingly linked to the onset and progression of the disease, paving the way for potential microbiome-targeted therapies.
Understanding Ulcerative Colitis: Continuous Mucosal Inflammation
Ulcerative colitis (UC) is another form of IBD, but it is characterized by continuous inflammation that primarily affects the innermost lining (mucosa) of the colon and rectum. The inflammation typically begins in the rectum and extends proximally throughout the colon. Unlike Crohn’s, UC does not typically involve the deeper layers of the intestinal wall or cause skip lesions, though severe cases can lead to toxic megacolon. Symptoms include bloody diarrhea, abdominal pain, and urgency.
Technological Innovations in UC Research and Diagnosis:
- High-Resolution Endoscopy and Chromoendoscopy: Modern endoscopes provide high-definition imaging, allowing for better visualization of mucosal abnormalities. Chromoendoscopy, which involves spraying dyes onto the colon surface, enhances the detection of subtle inflammatory changes, polyps, and precancerous lesions, which are a concern in long-standing UC. Confocal laser endomicroscopy offers even higher magnification, enabling in-vivo cellular-level examination of the colonic mucosa.
- Biomarker Discovery: Technological advancements in laboratory diagnostics are crucial for identifying reliable biomarkers for UC. Highly sensitive assays are used to detect inflammatory markers in blood and stool, such as C-reactive protein (CRP) and fecal calprotectin. Fecal calprotectin, in particular, has emerged as a non-invasive indicator of intestinal inflammation, aiding in diagnosis, monitoring disease activity, and predicting treatment response.
- Artificial Intelligence in Pathology: The interpretation of biopsies is a critical step in diagnosing and grading UC. AI algorithms are being developed to assist pathologists in analyzing tissue samples, identifying inflammatory infiltrates, and assessing the severity of mucosal damage with increased accuracy and consistency. This can lead to more objective and reproducible diagnoses.
The Technological Frontier in Diagnosis and Monitoring
Accurate and timely diagnosis, coupled with consistent monitoring of disease activity, are paramount for effectively managing IBD. Technology plays an indispensable role in refining these processes, offering less invasive, more precise, and more patient-centric approaches.

Enhancing Diagnostic Precision
The distinction between Crohn’s disease and ulcerative colitis, as well as the identification of specific disease phenotypes and severity, can be challenging. Technological innovations are bridging these diagnostic gaps.
- AI-Assisted Diagnostic Tools: Machine learning models are being trained on vast datasets of patient information, including clinical symptoms, imaging scans, genetic data, and histopathology. These AI tools can assist clinicians in differentiating between Crohn’s and UC, predicting disease progression, and identifying patients at higher risk of complications. For instance, AI could analyze patterns in medical records or endoscopic images to flag potential IBD cases for further investigation.
- Point-of-Care Testing: The development of rapid diagnostic tests that can be performed at the point of care is a significant technological advancement. While still evolving for IBD, the concept of portable devices that can quickly analyze blood or stool for inflammatory markers could revolutionize outpatient management, allowing for immediate assessment of disease flares without the need for extensive laboratory processing.
- Digital Pathology and Telemedicine: Digitalization of pathology slides allows for remote consultation and expert review, improving diagnostic accuracy, especially in resource-limited settings. Telemedicine platforms, enhanced by secure data sharing and high-resolution imaging, are also enabling remote patient monitoring and virtual consultations, increasing access to specialist care for individuals with IBD.
Continuous Monitoring and Personalized Management
Chronic diseases like IBD require ongoing monitoring to assess treatment efficacy, detect flares early, and adjust therapy as needed. Technology is enabling a shift towards more proactive and personalized management strategies.
- Wearable Sensors and Remote Patient Monitoring: While not yet widespread for IBD, the potential of wearable sensors is significant. Devices that can track physiological parameters like heart rate, body temperature, and potentially even gut motility or subtle changes in hydration could provide continuous, real-time data on a patient’s health status. This data can be transmitted to healthcare providers, enabling early detection of flares and proactive interventions.
- Digital Health Platforms and Apps: Numerous mobile applications and digital health platforms are emerging to help patients manage their IBD. These tools can facilitate symptom tracking, medication reminders, diet logging, and communication with healthcare teams. Data collected through these platforms can provide valuable insights into disease patterns and treatment effectiveness, empowering patients to take a more active role in their care.
- Predictive Analytics: By integrating data from various sources—genomic profiles, lifestyle factors, treatment history, and real-time monitoring—predictive analytics can be employed to forecast individual patient responses to different therapies, predict the likelihood of flares, and identify patients who may benefit from more aggressive treatment strategies. This move towards precision medicine is heavily reliant on sophisticated data processing and analytical technologies.
The Future of IBD: Technology-Driven Therapeutics and Research
The technological revolution is not only transforming how we diagnose and monitor IBD but also profoundly impacting the development of new therapeutic strategies and the fundamental understanding of disease mechanisms.
Novel Therapeutic Approaches
The limitations of current treatments for Crohn’s disease and ulcerative colitis are driving innovation in therapeutic development, with technology playing a central role.
- Precision Biologics and Gene Therapy: Biologic therapies, which target specific components of the immune system involved in inflammation, have revolutionized IBD treatment. Advanced biotechnological techniques are enabling the development of more targeted biologics with fewer side effects. Furthermore, the burgeoning field of gene therapy holds promise for correcting underlying genetic defects or modulating immune responses at a cellular level, though this remains largely in the experimental stages for IBD.
- Drug Delivery Systems: Innovations in drug delivery aim to improve the efficacy and reduce the systemic side effects of IBD medications. This includes developing targeted delivery systems that release medication directly to the inflamed areas of the gut, such as smart capsules or nanoparticles. Advanced polymer science and nanotechnology are key enablers of these innovations.
- AI in Drug Discovery: Artificial intelligence is accelerating the drug discovery process by analyzing vast molecular databases, predicting the efficacy and safety of potential drug candidates, and optimizing molecular structures. This can significantly reduce the time and cost associated with bringing new IBD therapies to market.
Unraveling Complex Pathogenesis
The chronic and multifactorial nature of IBD presents a significant research challenge. Technological advancements are providing powerful tools to unravel these complexities.
- Organ-on-a-Chip Technology: Microfluidic devices that mimic the structure and function of human organs, such as the gut-on-a-chip, are revolutionizing preclinical research. These models allow scientists to study the interactions between immune cells, intestinal epithelial cells, the microbiome, and specific pathogens in a controlled environment, providing more accurate disease modeling than traditional cell cultures.
- Single-Cell Analysis: Technologies like single-cell RNA sequencing allow researchers to analyze the gene expression profiles of individual cells within the inflamed gut. This provides an unprecedented resolution for understanding cellular heterogeneity, identifying specific immune cell subsets driving inflammation, and pinpointing cellular mechanisms of disease.
- Computational Modeling and Simulation: Sophisticated computational models are being used to simulate the complex biological systems involved in IBD. These simulations can help researchers understand how genetic, environmental, and immunological factors interact to trigger and sustain inflammation, leading to new hypotheses and research directions.
In conclusion, Crohn’s disease and ulcerative colitis are multifaceted inflammatory bowel diseases that present significant challenges for diagnosis, management, and treatment. However, the relentless march of technological innovation is providing us with powerful new tools. From advanced imaging and AI-assisted diagnostics to precision biologics and sophisticated research platforms, technology is not merely augmenting our capabilities; it is fundamentally transforming our understanding and approach to these chronic conditions. As we continue to harness the potential of these innovations, the future holds significant promise for improved patient outcomes and a deeper comprehension of the intricate mechanisms underlying inflammatory bowel diseases.
