The human body is a marvel of intricate engineering, with a complex network of bones, muscles, and nerves working in harmony to facilitate movement. At the core of this system lies the spine, a pillar of support that enables us to stand tall and navigate the world. Within the spine, intervertebral discs act as shock absorbers, cushioning the vertebrae and allowing for flexibility. However, these vital components are not immune to injury, and a common ailment that affects them is a slipped disc, also known as a herniated or ruptured disc. Understanding what a slipped disc feels like is crucial for seeking timely medical attention and managing this often debilitating condition.
The Anatomy of a Slipped Disc
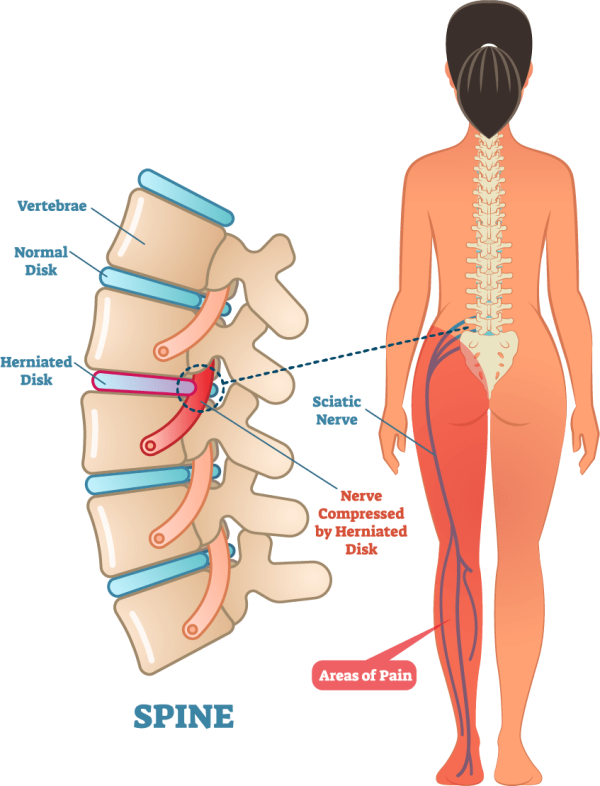
To truly grasp the sensation of a slipped disc, it’s essential to understand its underlying cause and the spinal anatomy involved. The spine is comprised of a series of bones called vertebrae, stacked one upon the other. Between each vertebra lies an intervertebral disc, a donut-shaped structure with a softer, gel-like center (nucleus pulposus) encased in a tougher, rubbery outer layer (annulus fibrosus). These discs are designed to withstand significant pressure and act as shock absorbers, preventing the vertebrae from grinding against each other.
The Discs: Cushions Under Pressure
Imagine these discs as jelly-filled doughnuts. The annulus fibrosus is the tough outer dough, providing structural integrity and containing the soft, gelatinous nucleus pulposus within. This design allows the spine to bend, twist, and absorb the impact of daily activities like walking, running, and jumping. Over time, or due to injury, the annulus fibrosus can weaken or tear. When this happens, the soft nucleus pulposus can bulge outwards, or even push through the tear, leading to a herniation. This displaced material can then press on nearby spinal nerves.
Spinal Nerves: The Body’s Communication Highway
The spinal cord, a bundle of nerves extending from the brain down the back, sends and receives signals that control everything from voluntary movements to sensory perception. Branching off from the spinal cord at various levels are the spinal nerves, which extend to different parts of the body. These nerves are incredibly sensitive, and even slight pressure can disrupt their function, leading to a cascade of uncomfortable sensations. When a slipped disc irritates or compresses a spinal nerve, it can trigger a range of symptoms that can be quite alarming.
The Spectrum of Pain and Discomfort
The feeling of a slipped disc is not a singular sensation but rather a spectrum of pain and discomfort that can vary greatly depending on the location, size, and degree of nerve compression. While some individuals may experience mild, intermittent discomfort, others can suffer from severe, incapacitating pain. The type of pain, its intensity, and its accompanying symptoms are all key indicators that can help identify this condition.
Localized Back Pain: The Initial Warning
Often, the first sign of a slipped disc is localized pain in the back. This pain might feel like a dull ache or a sharp, stabbing sensation. It can be constant or come and go, and it might be aggravated by certain movements, such as bending, lifting, or twisting. The location of this back pain can provide a clue to which disc is affected. For instance, a slipped disc in the lower back (lumbar spine) will typically cause pain in the lower back, while a disc issue in the neck (cervical spine) will manifest as neck pain. This initial discomfort serves as a crucial warning sign that something is amiss within the spinal column.
Radiating Pain: The Nerve’s Cry for Help
Perhaps the most distinctive symptom of a slipped disc is radiating pain, often referred to as sciatica when it originates from a herniated disc in the lower back. This pain travels along the path of the affected nerve, extending beyond the immediate area of the spine. If a nerve root in the lumbar spine is compressed, the pain can radiate down the buttock, through the thigh, and even into the calf and foot. Similarly, a slipped disc in the cervical spine can cause pain that travels down the arm, into the hand, and through the fingers. This radiating pain is often described as sharp, burning, or electric-shock-like, a testament to the nerve being directly impinged upon.
Numbness and Tingling: The Communication Breakdown
Beyond pain, nerve compression from a slipped disc can also lead to a loss of sensation or abnormal sensations in the areas served by the affected nerve. This can manifest as numbness, a feeling of pins and needles (paresthesia), or even a crawling sensation under the skin. The affected area might feel “asleep” or have a reduced ability to feel touch, temperature, or pressure. This disruption in nerve signaling highlights the compromised communication between the brain and the body, a direct consequence of the disc’s encroachment on the nerve.
Weakness: The Motor Control Impairment

In more severe cases of nerve compression, a slipped disc can affect the motor functions controlled by the compromised nerve. This can result in muscle weakness in the affected limb. For example, a herniated disc in the lower back might lead to weakness in the leg, making it difficult to lift the foot (foot drop) or stand on the toes. Similarly, cervical disc herniation can cause weakness in the arm or hand, impacting grip strength or the ability to perform fine motor tasks. This weakness is a clear indication that the nerve’s ability to transmit signals to the muscles has been significantly impaired.
Factors Influencing the Sensation
The experience of a slipped disc is not uniform; several factors can influence how it feels. These variables range from the individual’s physiology to the specific characteristics of the herniation itself. Understanding these nuances can help individuals better describe their symptoms to healthcare professionals, leading to a more accurate diagnosis and effective treatment plan.
Location, Location, Location: Cervical, Thoracic, and Lumbar Disc Herniation
The primary determinant of where and how a slipped disc is felt is its location within the spine.
- Cervical Spine (Neck): Herniation in the neck can cause pain, numbness, or tingling in the neck, shoulders, arms, and hands. It can also lead to headaches and neck stiffness.
- Thoracic Spine (Mid-Back): While less common, herniated discs in the mid-back can cause pain in the chest, abdomen, or back. This can sometimes be mistaken for cardiac or digestive issues.
- Lumbar Spine (Lower Back): This is the most frequent site for disc herniation, typically causing pain in the lower back that radiates down one or both legs (sciatica), along with numbness, tingling, or weakness in the legs and feet.
Size and Direction of Herniation: The Degree of Pressure
The size of the herniated portion of the disc and the direction in which it protrudes play a significant role in the severity of symptoms. A small bulge might cause minimal irritation, while a large extrusion can press on multiple nerve roots, leading to more widespread and intense symptoms. The direction of the bulge is also critical. If it protrudes directly onto a nerve root, the pain and neurological deficits will be more pronounced than if it protrudes centrally.
Individual Pain Thresholds and Nerve Sensitivity: Personal Differences
It’s important to acknowledge that individuals have varying pain thresholds and levels of nerve sensitivity. What one person experiences as unbearable pain, another might tolerate with less distress. Furthermore, the individual’s overall health, activity level, and any pre-existing neurological conditions can influence how a slipped disc manifests. This variability underscores the importance of a thorough medical evaluation rather than relying solely on self-diagnosis based on reported symptoms.
When to Seek Medical Attention
Recognizing the potential signs of a slipped disc and understanding what it might feel like is the first step towards effective management. However, it is crucial to emphasize that this article is for informational purposes only and does not substitute for professional medical advice. If you are experiencing persistent or severe back pain, radiating pain, numbness, tingling, or weakness in your limbs, it is imperative to consult a healthcare professional for an accurate diagnosis and appropriate treatment.
Red Flags: Urgent Symptoms to Watch For
Certain symptoms associated with a slipped disc warrant immediate medical attention. These are often referred to as “red flags” and can indicate a more serious condition, such as cauda equina syndrome, a medical emergency. These red flags include:
- Loss of bowel or bladder control: This is a critical sign that requires urgent evaluation.
- Numbness or tingling in the saddle area: This refers to the area of the body that would sit on a saddle, including the groin and inner thighs.
- Severe or progressive weakness: If leg weakness is rapidly worsening, it necessitates immediate medical assessment.
- Pain that is not relieved by rest: Persistent, severe pain that doesn’t improve even when lying down can be a cause for concern.
The Diagnostic Process: From Symptoms to Solutions
Upon experiencing concerning symptoms, a healthcare provider will typically begin with a thorough medical history and physical examination. They will ask detailed questions about the nature of your pain, its location, duration, and any aggravating or relieving factors. During the physical exam, they will assess your range of motion, muscle strength, reflexes, and sensation. Depending on the findings, imaging tests such as X-rays, MRI scans, or CT scans may be ordered to visualize the spine and confirm the diagnosis of a slipped disc.

Treatment Options: Managing the Condition
Once a slipped disc is diagnosed, a range of treatment options are available, tailored to the individual’s specific needs and the severity of their condition. These can include conservative treatments such as pain medication, anti-inflammatory drugs, physical therapy, and activity modification. In more severe cases, or when conservative treatments are not effective, surgical intervention may be considered. The goal of treatment is to alleviate pain, restore function, and prevent long-term complications. Understanding the symptoms and seeking timely medical care are essential components in navigating the challenges presented by a slipped disc.
