The delicate skin beneath our eyes is often the first to show signs of aging, stress, or underlying health concerns. While fine lines and dark circles are common culprits, a less frequently discussed but equally bothersome issue is the appearance of small, pearly white bumps. These are commonly known as milia, and they can be a persistent source of frustration for those seeking a smooth, clear complexion. Understanding what causes milia, how they differ from other common under-eye concerns, and the most effective treatment and prevention strategies is key to addressing them.
Understanding Milia: The Science Behind Those Tiny Bumps
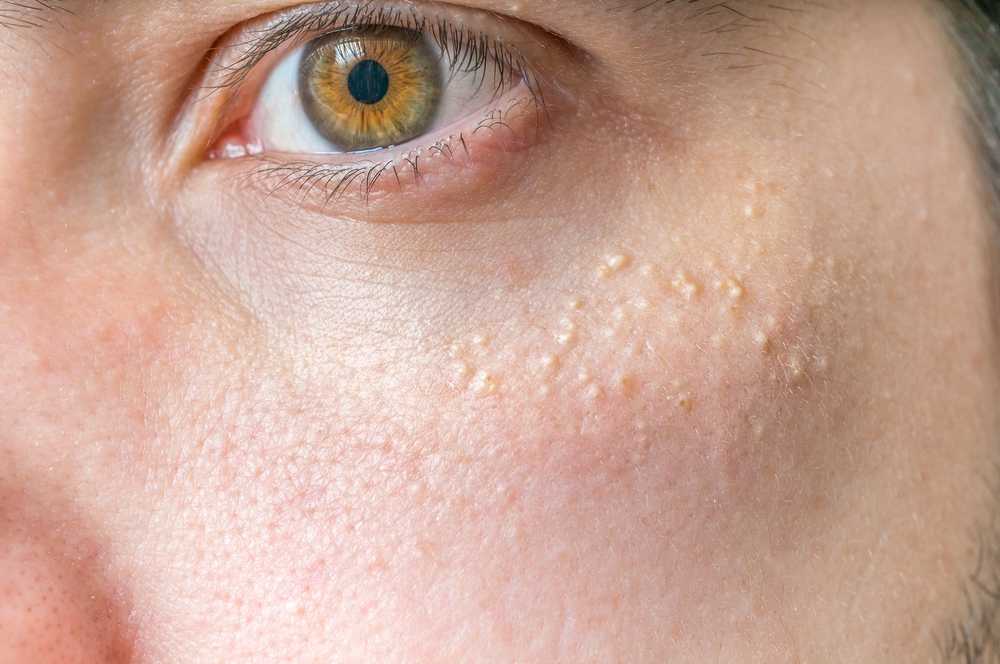
Milia are tiny, benign cysts that typically appear as small, white or yellowish bumps on the skin. They are essentially trapped keratin, a protein that makes up our hair, skin, and nails. When dead skin cells fail to shed properly and become trapped beneath the surface of the skin, they can form these characteristic small cysts. Unlike acne, milia do not have an opening to the skin’s surface and are therefore not inflamed or infected. They are most common on the face, particularly around the eyes and on the cheeks, but can appear elsewhere on the body.
Types of Milia and Their Underlying Causes
While the fundamental mechanism of trapped keratin remains consistent, milia can manifest in different forms and often have distinct contributing factors. Recognizing these nuances is crucial for effective management.
Primary Milia: A Natural Occurrence
Primary milia are the most common type and occur spontaneously. They develop when dead skin cells and keratin become trapped in tiny pockets just below the skin’s surface. This is particularly prevalent in infants, where their skin is still developing its natural exfoliation processes. However, primary milia can also occur in adults due to a variety of factors that disrupt normal skin shedding. These can include sun damage, which thickens the skin’s outer layer and impedes exfoliation, and the natural aging process, which can slow down cell turnover. In some cases, genetic predisposition may also play a role in an individual’s susceptibility to developing primary milia.
Secondary Milia: A Consequence of Skin Damage
Secondary milia, on the other hand, arise as a result of damage to the skin. This damage can stem from various sources. Certain skin conditions, such as blistering diseases like epidermolysis bullosa or porphyria cutanea tarda, can cause the skin to blister and peel, leading to the obstruction of hair follicles and the formation of milia. Furthermore, injuries to the skin, including burns, severe sunburns, or even extensive cosmetic procedures like dermabrasion or laser resurfacing, can disrupt the skin’s normal shedding process, resulting in secondary milia. Products applied to the skin can also contribute. Heavy, occlusive skincare products, particularly those containing petrolatum or thick oils, can clog pores and hinder exfoliation, thereby promoting the development of secondary milia.
Neonatal Milia: A Transient Phenomenon
Neonatal milia are a specific type of primary milia that affect newborns. These appear as tiny white bumps on the nose, chin, or cheeks of a baby. They are extremely common, affecting approximately 40-50% of all newborns. The exact cause of neonatal milia is not fully understood, but it is believed to be related to the immature development of the sebaceous glands and the skin’s exfoliation processes in infants. The good news is that neonatal milia are almost always transient and typically disappear on their own within a few weeks to months after birth, without requiring any treatment. They are harmless and do not cause any discomfort to the baby.
Differentiating Milia from Other Under-Eye Concerns
The appearance of small white dots under the eyes can sometimes be confused with other common skin conditions, leading to incorrect self-diagnosis and treatment. It’s important to distinguish milia from these other issues to ensure appropriate care.
Distinguishing Milia from Acne and Pimples
While both milia and acne involve bumps on the skin, their fundamental nature and treatment differ significantly. Acne, or pimples, are a result of inflamed hair follicles infected with bacteria. They typically present as red, swollen bumps that can contain pus and are often painful. The key difference is that acne lesions have an open pore that can become infected, whereas milia are closed cysts with no connection to the surface. Acne also typically involves the presence of blackheads and whiteheads, which are open and closed comedones, respectively. Milia, on the other hand, are uniformly small, hard, pearly white bumps. Attempting to “pop” milia is generally ineffective and can lead to scarring or infection, unlike acne, where extraction of a mature pimple can sometimes be beneficial under sterile conditions.
Milia vs. Syringomas and Skin Tags
Beyond acne, milia can also be mistaken for other benign skin growths like syringomas and skin tags, particularly in the under-eye area. Syringomas are benign tumors of the sweat glands that typically appear as small, flesh-colored or yellowish papules, often in clusters around the eyes. They tend to be softer than milia and may have a slightly translucent quality. Skin tags, on the other hand, are small, soft, flesh-colored growths that hang off the skin. They are usually attached by a stalk and are more common in areas where skin rubs against skin, such as the neck or underarms, though they can occasionally appear on the face. The distinct texture, color, and growth pattern help differentiate these conditions from the solid, pearly white appearance of milia.

Treatment and Prevention Strategies for Milia
Fortunately, milia are generally harmless and often resolve on their own. However, for those who find them aesthetically bothersome, several effective treatment and prevention strategies are available. The approach chosen will often depend on the severity and persistence of the milia.
Professional Treatments: Extraction and Therapies
When milia prove persistent or extensive, professional intervention is often the most effective route. Dermatologists and qualified skincare professionals have access to a range of treatments designed to safely and efficiently remove milia.
Manual Extraction by a Professional
The most common and direct method for removing milia is manual extraction performed by a trained professional. Using a sterile lancet or needle, the dermatologist will carefully create a tiny opening in the skin over the milia. This allows for the gentle expression of the trapped keratin with a comedone extractor. It’s crucial that this procedure is performed by a professional to minimize the risk of infection, scarring, or hyperpigmentation. Attempting to extract milia at home with unsterilized equipment is strongly discouraged due to these potential complications.
Chemical Peels and Microdermabrasion
Chemical peels and microdermabrasion are exfoliating treatments that can be highly effective in managing milia, particularly when they are widespread or recurrent. Chemical peels involve applying a solution to the skin that exfoliates the outer layers, promoting cell turnover and helping to dislodge trapped keratin. The strength of the peel can be adjusted based on the individual’s skin type and sensitivity. Microdermabrasion, on the other hand, uses a device to gently abrade the outermost layer of skin, removing dead skin cells and revealing smoother, fresher skin beneath. Both treatments, when performed by a qualified practitioner, can help prevent the formation of new milia by improving the skin’s natural exfoliation process.
Prescription Topical Treatments
In some cases, topical medications prescribed by a dermatologist can help manage milia. Retinoids, such as tretinoin or adapalene, are particularly useful. These vitamin A derivatives work by increasing cell turnover and preventing the buildup of keratin within hair follicles. They can be applied directly to the affected areas and, over time, help to reduce the appearance of existing milia and prevent new ones from forming. However, retinoids can cause initial irritation, dryness, and sun sensitivity, so their use should be supervised by a healthcare professional.
At-Home Care and Prevention Tips
While professional treatments offer the most definitive solutions for existing milia, consistent at-home care plays a vital role in prevention and in managing milder cases.
Gentle Exfoliation and Cleansing
The cornerstone of milia prevention is maintaining a consistent and gentle exfoliation routine. Opt for a mild chemical exfoliant containing ingredients like alpha-hydroxy acids (AHAs) or beta-hydroxy acids (BHAs). Glycolic acid and salicylic acid are excellent choices for promoting cell turnover and preventing pore blockage. A gentle physical exfoliant, such as a soft brush or a finely granulated scrub, can also be used sparingly. Crucially, cleansing should be thorough but gentle, removing makeup and impurities without stripping the skin of its natural oils. Over-washing or using harsh cleansers can actually exacerbate dryness and lead to increased keratin buildup.
Sun Protection is Paramount
Sun damage is a significant contributor to the thickening of the skin’s outer layer, which impedes proper exfoliation and can lead to the formation of milia. Therefore, diligent sun protection is paramount. Every day, regardless of the weather, apply a broad-spectrum sunscreen with an SPF of 30 or higher to all exposed skin, including the under-eye area. Reapply every two hours when outdoors, especially after swimming or sweating. Wearing sunglasses and a wide-brimmed hat can provide additional protection against harmful UV rays.

Skincare Product Selection and Routine
The products you choose for your under-eye area can either contribute to or help prevent milia. Avoid heavy, occlusive creams and oils that can clog pores. Instead, opt for lightweight, non-comedogenic formulations. Ingredients like hyaluronic acid can provide hydration without greasiness, while antioxidants like vitamin C can help protect the skin from environmental damage. Always remove makeup thoroughly before bed. Consider incorporating a gentle eye serum designed to promote cell turnover or hydration into your routine. A consistent skincare regimen that prioritizes gentle exfoliation, thorough cleansing, and diligent sun protection is your best defense against the persistent appearance of milia.
