Pain in the back of the knee, medically known as posterior knee pain, is a common complaint that can significantly impact an individual’s mobility and quality of life. Understanding the underlying causes, potential symptoms, and effective management strategies is crucial for effective treatment and recovery. This debilitating discomfort can stem from a variety of issues, ranging from minor strains to more complex medical conditions.
Causes of Posterior Knee Pain
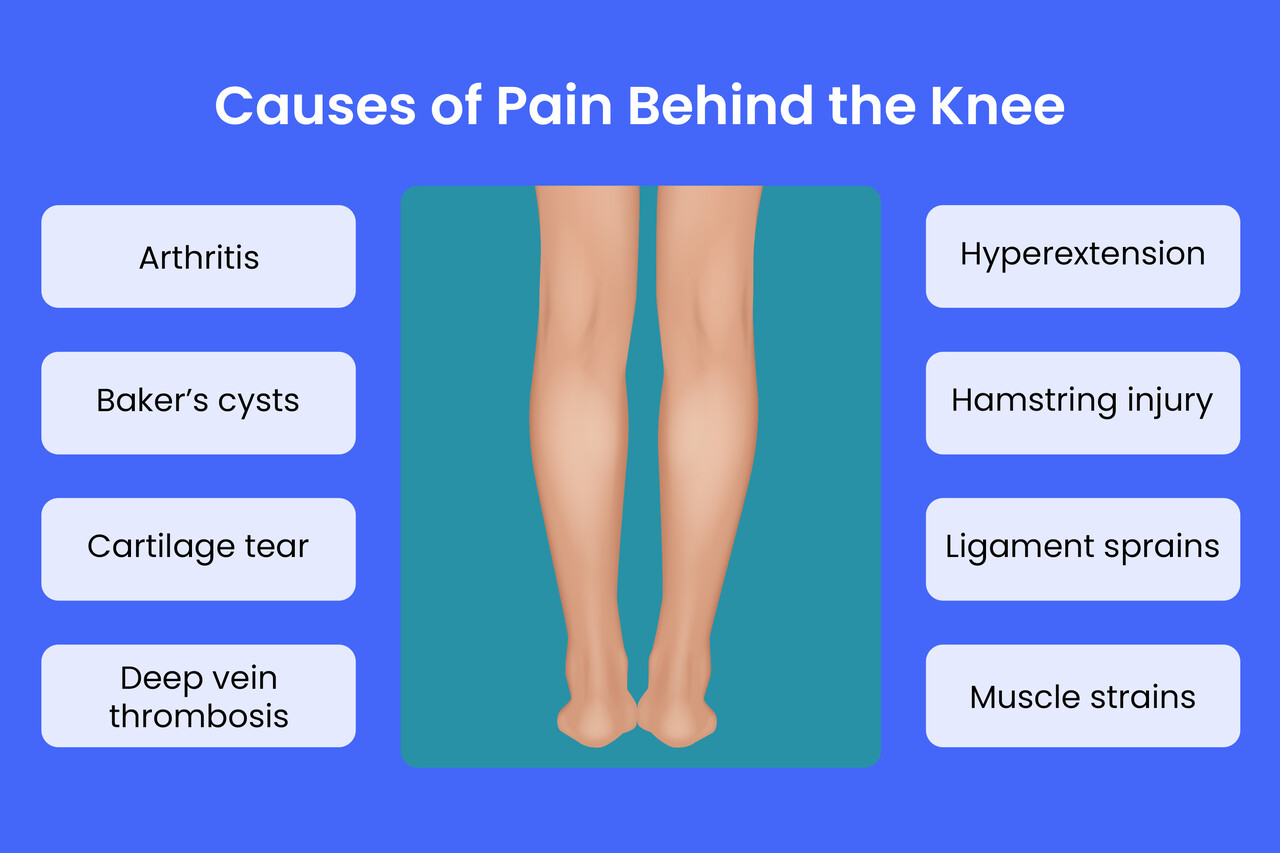
Several factors can contribute to pain in the back of the knee. These can be broadly categorized into injuries, overuse conditions, and anatomical abnormalities.
Injuries
Acute injuries are a frequent cause of posterior knee pain. These can include:
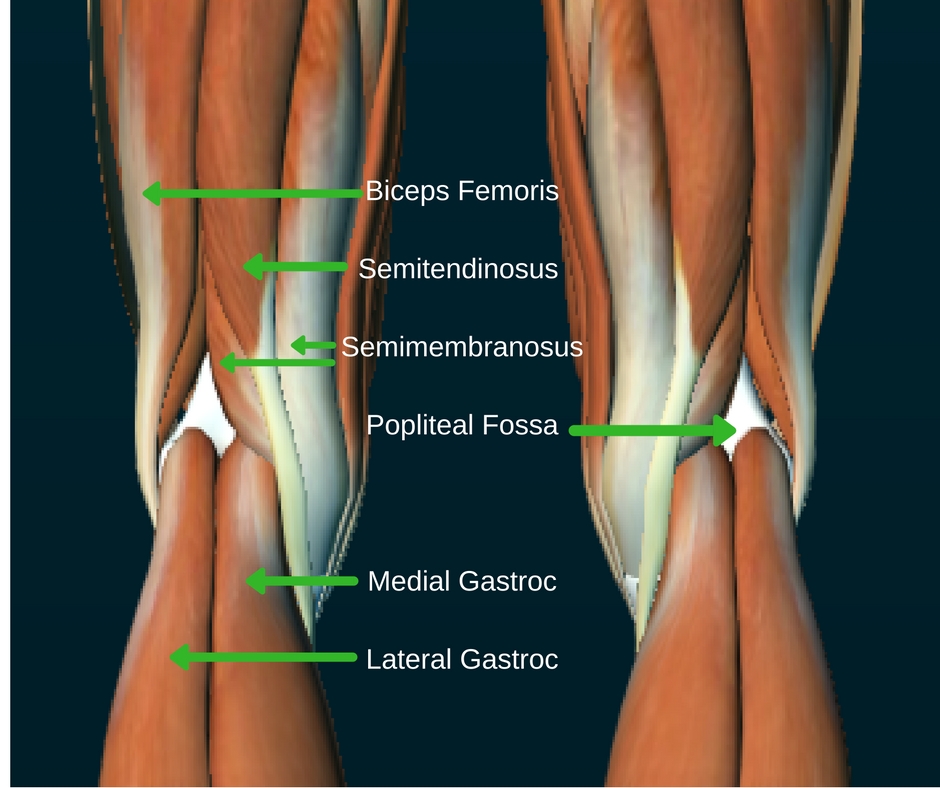
- Hamstring Tendon Strain or Tear: The hamstring muscles run along the back of the thigh and their tendons attach to the bones in the back of the knee. Overstretching or sudden forceful contraction of these muscles can lead to a strain or even a tear of the tendon. This often results in immediate pain, swelling, and tenderness in the back of the knee. The severity can range from a mild pull to a complete rupture. Factors such as insufficient warm-up before exercise, sudden increases in activity intensity, or poor flexibility can predispose individuals to hamstring injuries.
- Gastrocnemius Muscle Strain or Tear: The gastrocnemius is the larger of the two calf muscles, and its upper part is located in the back of the lower leg, just above the knee joint. A strain or tear in this muscle can cause pain that radiates into the back of the knee. This is often referred to as a “tennis leg” injury and can occur during activities that involve sudden bursts of speed, jumping, or forceful push-offs, like sprinting or tennis.
- Posterior Cruciate Ligament (PCL) Sprain or Tear: The PCL is one of the four major ligaments in the knee, located at the back of the joint. It plays a vital role in stabilizing the knee, particularly against backward movement of the tibia (shinbone). A PCL injury typically occurs from a direct blow to the front of the tibia when the knee is bent, such as in a dashboard injury during a car accident or a direct impact during contact sports like football. Symptoms include a popping sensation at the time of injury, immediate pain, swelling, and a feeling of instability in the knee.
- Meniscus Tear: The menisci are C-shaped pieces of cartilage that act as shock absorbers between the thighbone (femur) and shinbone (tibia). While tears often occur in the inner or outer part of the meniscus, a posterior horn tear of the medial or lateral meniscus can present with pain at the back of the knee. These tears can be caused by twisting or rotational injuries to the knee, or can develop gradually over time due to wear and tear. Pain may be accompanied by clicking, locking, or catching sensations within the knee joint.
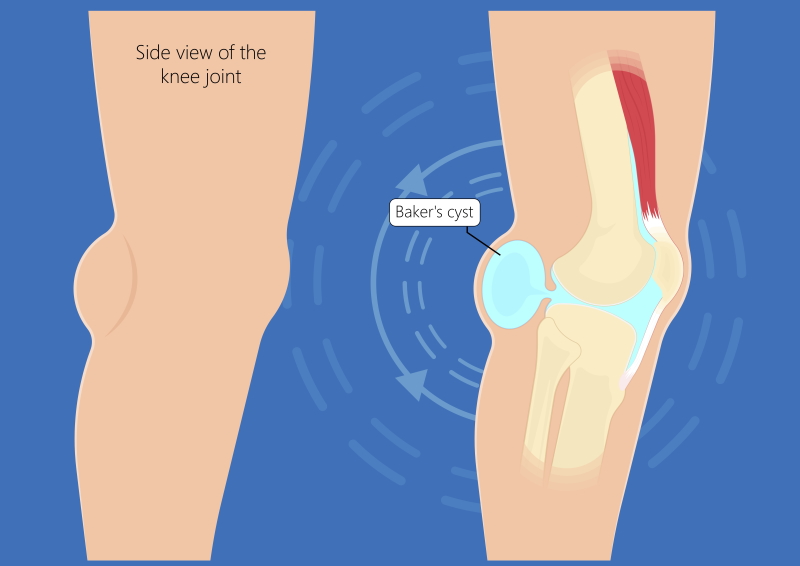
- Baker’s Cyst (Popliteal Cyst): This is a fluid-filled sac that forms on the back of the knee. It occurs when excess synovial fluid, the lubricating fluid within the knee joint, is pushed out into the space behind the knee. Baker’s cysts are often a secondary condition, meaning they are usually caused by another underlying knee problem such as arthritis, meniscus tears, or ligament injuries that increase the production of synovial fluid. The cyst itself can cause a feeling of fullness, tightness, and aching pain in the back of the knee, especially when the knee is fully extended or bent. In some cases, a Baker’s cyst can rupture, leading to sudden, sharp pain that can mimic a calf muscle tear.
Overuse Conditions
Repetitive stress and overuse can lead to conditions that manifest as posterior knee pain, even without a specific traumatic event.
- Patellofemoral Pain Syndrome (PFPS): While typically associated with pain at the front of the knee, PFPS can sometimes present with pain that refers to the back of the knee. This condition involves pain around or behind the kneecap, often exacerbated by activities like climbing stairs, squatting, or prolonged sitting with a bent knee. It’s often caused by overuse, muscle imbalances (weak quadriceps or hip abductors), or issues with the tracking of the kneecap.
- Iliotibial (IT) Band Syndrome: The IT band is a thick band of fibrous tissue that runs along the outside of the thigh, from the hip to just below the knee. While IT band syndrome is more commonly felt on the outside of the knee, in some cases, tightness and inflammation of the IT band can cause referred pain to the posterior aspect of the knee, especially during or after repetitive activities like running or cycling.
- Tendinitis: Inflammation of the tendons around the knee can cause pain. While anterior tendinitis (e.g., patellar tendinitis or “jumper’s knee”) is more common, inflammation of the hamstring tendons (hamstring tendinopathy) or even the popliteal tendon (a small tendon located in the back of the knee that helps with knee flexion and rotation) can lead to posterior knee pain. This is often due to overuse, improper training techniques, or inadequate rest.
Anatomical Abnormalities and Other Conditions
Certain anatomical variations or underlying medical conditions can also contribute to posterior knee pain.
- Osteoarthritis: Degenerative joint disease, or osteoarthritis, can affect any part of the knee joint, including the posterior compartment. As the cartilage wears away, bone rubs against bone, leading to pain, stiffness, and reduced mobility. Pain associated with osteoarthritis may be worse with activity and improve with rest, but can also be present at rest in more advanced stages.
- Referred Pain: Sometimes, pain originating from other areas can be felt in the back of the knee. For instance, problems in the lower back, such as a herniated disc or spinal stenosis, can cause nerve compression that leads to pain radiating down the leg, including the back of the knee. Hip joint problems, like hip osteoarthritis or bursitis, can also refer pain to the knee.
- Vascular Issues: In rare cases, vascular problems can cause posterior knee pain. Popliteal artery entrapment syndrome, where the popliteal artery (located behind the knee) is compressed by surrounding muscles or ligaments, can lead to claudication (pain, cramping, or fatigue) in the calf and back of the knee during exercise that subsides with rest. Deep vein thrombosis (DVT), a blood clot in a deep vein, can also cause pain, swelling, and warmth in the calf and potentially the back of the knee.
Symptoms of Posterior Knee Pain
The specific symptoms associated with pain in the back of the knee can vary depending on the underlying cause. However, some common symptoms include:
Pain and Discomfort
- Aching or Dull Pain: This is a common symptom, often described as a persistent, deep ache that can worsen with activity or prolonged standing.
- Sharp or Stabbing Pain: This type of pain is often indicative of an acute injury, such as a ligament tear, meniscus tear, or muscle rupture. It may occur suddenly during an activity.
- Burning Sensation: A burning sensation can sometimes be related to nerve irritation or inflammation.
- Throbbing Pain: This may be associated with inflammation or vascular issues.
Stiffness and Limited Range of Motion
- Difficulty Bending or Straightening the Knee: Many individuals with posterior knee pain experience a restricted range of motion, making it challenging to fully flex or extend the knee. This stiffness can be particularly noticeable after periods of rest or upon waking.
- Tightness in the Back of the Knee: A feeling of tightness or a pulling sensation in the back of the knee is a common complaint, often associated with hamstring or calf muscle involvement, or a Baker’s cyst.
Swelling and Inflammation
- Visible Swelling: Swelling behind the knee can be indicative of inflammation, fluid accumulation (as in a Baker’s cyst), or bleeding from an injury. The swelling may fluctuate depending on activity levels.
- Warmth: An area of warmth in the back of the knee can suggest inflammation or infection, though it’s more commonly associated with inflammation from injury or overuse.
Instability and Giving Way
- Feeling of Instability: Some individuals describe a sensation of the knee “giving way” or feeling unstable, particularly when bearing weight or during certain movements. This is a hallmark symptom of ligamentous injuries, such as a PCL tear.
- Clicking, Popping, or Grinding Sensations: These sounds, often accompanied by pain, can suggest damage to the menisci or cartilage within the knee joint.
Other Associated Symptoms
- Tenderness to Touch: The affected area in the back of the knee may be tender to palpation, indicating localized inflammation or injury.
- Pain with Specific Activities: Pain is often exacerbated by activities that stress the posterior structures of the knee, such as running, jumping, squatting, climbing stairs, or prolonged sitting with the knee bent.
It’s important to note that the combination and intensity of these symptoms can provide valuable clues to the underlying cause of posterior knee pain. For example, a sudden onset of sharp pain and swelling after a twisting injury might point towards a meniscus tear or ligament injury, while a gradual onset of dull aching pain with stiffness might suggest osteoarthritis or tendinopathy.
Diagnosis and Treatment of Posterior Knee Pain
Accurate diagnosis is the cornerstone of effective treatment for posterior knee pain. A thorough evaluation by a healthcare professional, typically a physician or physical therapist, is essential to identify the root cause.
Diagnostic Process
The diagnostic process usually involves a combination of the following:
- Medical History: The healthcare provider will ask detailed questions about the onset of pain, the nature of the pain, aggravating and alleviating factors, any specific injuries or activities that may have contributed, and the presence of other symptoms.
- Physical Examination: This involves a hands-on assessment of the knee. The provider will:
- Inspect: Look for any visible swelling, bruising, or deformities.
- Palpate: Gently press on different areas around the knee to identify points of tenderness and assess for warmth or swelling.
- Assess Range of Motion: Evaluate the active and passive range of motion of the knee, noting any limitations or pain during movement.
- Perform Special Tests: Conduct specific maneuvers designed to stress particular ligaments, tendons, or menisci to check for signs of injury. This might include tests for ligamentous laxity (e.g., posterior drawer test for PCL), meniscus integrity (e.g., McMurray test), and assessment of hamstring or calf muscle strength and flexibility.
- Imaging Studies: Depending on the suspected cause, imaging tests may be ordered:
- X-rays: Useful for visualizing bones and detecting conditions like osteoarthritis, fractures, or bone spurs.
- Magnetic Resonance Imaging (MRI): This is often the gold standard for visualizing soft tissues, including ligaments, tendons, menisci, and cartilage. An MRI can provide detailed images to confirm or rule out tears, inflammation, and other soft tissue abnormalities.
- Ultrasound: Can be helpful in assessing tendons, muscles, and fluid collections like Baker’s cysts.
- Arteriogram or Doppler Ultrasound: May be used if a vascular cause is suspected.
Treatment Strategies
Treatment for posterior knee pain is highly individualized and depends on the diagnosis. The primary goals are to reduce pain and inflammation, restore function, and prevent recurrence.
Non-Surgical Management
- RICE Protocol: For acute injuries, the RICE protocol (Rest, Ice, Compression, Elevation) is often recommended in the initial stages to manage pain and swelling.
- Rest: Avoiding activities that aggravate the pain.
- Ice: Applying ice packs to the affected area for 15-20 minutes several times a day.
- Compression: Using an elastic bandage or compression sleeve to reduce swelling.
- Elevation: Keeping the leg raised above heart level.
- Pain Management: Over-the-counter pain relievers like acetaminophen or non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen can help manage pain and inflammation. In some cases, stronger prescription medications may be necessary.
- Physical Therapy: This is a cornerstone of treatment for most causes of posterior knee pain. A tailored physical therapy program may include:
- Stretching Exercises: To improve flexibility of the hamstrings, calves, and quadriceps.
- Strengthening Exercises: To build strength in the muscles supporting the knee, including quadriceps, hamstrings, gluteals, and core muscles. Addressing muscle imbalances is often a key focus.
- Proprioception and Balance Training: To improve the knee’s stability and control.
- Manual Therapy: Techniques like massage and joint mobilization can help reduce muscle tension and improve joint mobility.
- Modalities: Ultrasound, electrical stimulation, or heat therapy may be used to aid in pain relief and tissue healing.
- Activity Modification: Temporarily modifying or avoiding activities that trigger pain is crucial to allow for healing. Gradually returning to activities once pain has subsided and function has improved is important.
- Orthotics and Bracing: In some cases, supportive braces or custom orthotics may be recommended to provide stability or correct biomechanical issues.
- Injections: Corticosteroid injections may be used to reduce inflammation in cases of significant inflammation, such as with a Baker’s cyst or tendinitis. Hyaluronic acid injections might be considered for osteoarthritis.
Surgical Intervention
Surgery is typically considered for posterior knee pain when non-surgical treatments have failed to provide relief or for severe injuries that require surgical repair. Surgical options depend on the specific condition and may include:
- Arthroscopy: A minimally invasive procedure used to diagnose and treat conditions like meniscus tears, ligament tears, or to debride inflamed tissues.
- Ligament Reconstruction: For significant PCL tears, surgical reconstruction may be necessary to restore knee stability.
- Meniscus Repair or Removal: Damaged portions of the meniscus can be repaired or surgically removed.
- Baker’s Cyst Excision: In persistent or symptomatic cases, a Baker’s cyst may be surgically removed, though addressing the underlying cause is paramount.
Prevention and Long-Term Management
Preventing posterior knee pain involves a proactive approach to maintaining knee health and addressing risk factors. Long-term management focuses on sustained healthy habits to minimize the risk of recurrence.
Preventive Measures
- Proper Warm-up and Cool-down: Always dedicate time to warm up muscles before engaging in physical activity and cool down afterwards. This helps prepare the muscles and tendons for stress and aids in recovery.
- Regular Stretching: Incorporate regular stretching exercises into your routine, paying particular attention to the hamstrings, quadriceps, and calf muscles. Improved flexibility can reduce the risk of strains.
- Gradual Progression of Activity: Avoid sudden increases in the intensity, duration, or frequency of exercise. Gradually build up your fitness levels to allow your body to adapt.
- Strength Training: Maintain a balanced strength training program that targets the muscles around the knee, hips, and core. Stronger muscles provide better support and stability to the knee joint.
- Proper Footwear: Wear appropriate and well-fitting footwear for your activities. Supportive shoes can help absorb shock and improve biomechanics.
- Maintain a Healthy Weight: Excess body weight places additional stress on the knee joint, increasing the risk of pain and injury.
- Listen to Your Body: Pay attention to any signs of pain or discomfort. Don’t push through significant pain, as this can worsen an injury. Allow for adequate rest and recovery.
- Good Biomechanics: Be mindful of your posture and movement patterns during daily activities and exercise. Correcting any faulty biomechanics, often with the help of a physical therapist, can reduce stress on the knee.
Long-Term Management Strategies
- Adherence to Exercise Programs: Continue with recommended stretching and strengthening exercises even after pain has resolved, as prescribed by a physical therapist or healthcare provider. Consistency is key to maintaining muscle balance and joint support.
- Activity Modification When Needed: Understand which activities aggravate your knee pain and learn to modify them or engage in alternative exercises that are less stressful on the knee.
- Weight Management: Continuing to maintain a healthy weight is crucial for long-term knee health, especially for individuals prone to or recovering from knee issues.
- Regular Check-ups: For individuals with chronic knee conditions like osteoarthritis, regular follow-up appointments with a healthcare provider are important to monitor the condition and adjust treatment plans as needed.
- Ergonomics: If your work or daily activities involve prolonged sitting, standing, or repetitive movements, consider ergonomic adjustments to minimize stress on your knees.
- Awareness of Warning Signs: Be aware of early warning signs of recurrence, such as mild aching, stiffness, or a feeling of tightness. Addressing these early can prevent a more significant flare-up.
By understanding the potential causes, recognizing the symptoms, seeking timely and accurate diagnosis, and diligently following a personalized treatment and prevention plan, individuals can effectively manage posterior knee pain and work towards regaining optimal knee function and an active lifestyle.
