The question of “what will Tramadol do to you” delves into the complex interplay between a pharmaceutical compound and the human body. While traditionally answered through clinical studies and pharmacological explanations, advancements in technology are increasingly offering new lenses through which to understand, predict, and even monitor the effects of medications like Tramadol. This article explores the technological frontiers that are shedding light on the multifaceted impact of Tramadol, from the molecular level to observable behavioral changes, and how innovation is shaping our understanding of its therapeutic benefits and potential risks.
The Neurological Landscape: Mapping Tramadol’s Impact with Advanced Imaging and AI
Tramadol, a synthetic opioid analgesic, exerts its effects by binding to mu-opioid receptors in the central nervous system, thereby inhibiting the reuptake of norepinephrine and serotonin. Understanding the precise neurological pathways and mechanisms involved is crucial for optimizing its use and mitigating adverse reactions. Technological innovations, particularly in neuroimaging and artificial intelligence, are revolutionizing our ability to visualize and analyze these intricate processes.
Functional Magnetic Resonance Imaging (fMRI) and Brain Activity
Functional Magnetic Resonance Imaging (fMRI) represents a cornerstone in non-invasively studying brain activity. By detecting changes in blood flow and oxygenation, fMRI allows researchers to identify which brain regions are activated or deactivated in response to stimuli or pharmacological agents. When investigating Tramadol, fMRI can reveal its impact on key areas associated with pain perception, mood regulation, and reward pathways. For instance, studies might employ fMRI to observe how Tramadol influences activity in the prefrontal cortex, amygdala, and anterior cingulate cortex, areas known to be involved in processing pain signals and emotional responses.
The application of fMRI in understanding Tramadol’s effects extends to identifying its influence on the limbic system, which plays a significant role in emotion and memory. Observing changes in connectivity between different brain regions while an individual is under the influence of Tramadol can provide insights into its potential to induce euphoria or dysphoria, and its contribution to psychological dependence. Furthermore, fMRI can help differentiate the neurological signatures of Tramadol from those of other analgesics, offering a more nuanced understanding of its unique pharmacological profile.
Computational Neuroscience and Predictive Modeling
Beyond static imaging, computational neuroscience is leveraging advanced algorithms and machine learning to build dynamic models of brain function and drug interactions. By feeding data from neuroimaging, genetic profiles, and patient-reported outcomes into sophisticated computational models, researchers can begin to predict individual responses to Tramadol. These models can account for a vast array of variables, including individual genetic predispositions, co-existing medical conditions, and other medications, all of which can influence how Tramadol is metabolized and how it affects the brain.
Machine learning algorithms, particularly deep learning networks, are adept at identifying complex, non-linear relationships within large datasets. This capability is invaluable in unraveling the intricate mechanisms by which Tramadol interacts with neurotransmitter systems and brain circuits. By analyzing patterns of neural activity, these models can potentially predict not only the analgesic efficacy of Tramadol for a given individual but also their susceptibility to side effects such as nausea, dizziness, or, in more severe cases, respiratory depression and serotonin syndrome. The predictive power of these computational approaches offers a promising avenue for personalized medicine, enabling clinicians to tailor Tramadol prescriptions for maximum benefit and minimal risk.
Physiological Monitoring: Wearable Tech and Biosensors for Real-time Insights
The effects of Tramadol are not confined to the brain; they manifest across a spectrum of physiological changes. The proliferation of wearable technology and sophisticated biosensors has opened up new possibilities for continuous, real-time monitoring of these physiological responses, offering a dynamic and objective complement to subjective patient reports.
Cardiovascular and Respiratory System Monitoring

Tramadol, like other opioids, can influence cardiovascular and respiratory functions. Heart rate, blood pressure, and breathing patterns can all be subtly altered. Modern wearable devices, such as smartwatches and fitness trackers equipped with advanced sensors, can continuously monitor heart rate variability and respiratory rate. For individuals prescribed Tramadol, these devices can provide a continuous stream of data that can alert healthcare providers to potential adverse events. Deviations from baseline heart rate or significant reductions in respiratory rate, when correlated with Tramadol use, can serve as early warning signs.
Beyond basic metrics, more advanced biosensors are being developed for continuous glucose monitoring, pulse oximetry, and even ECG monitoring. While not always integrated into consumer-grade wearables, these specialized sensors offer a more granular view of physiological status. For research purposes, or in clinical settings with heightened risk, continuous monitoring of oxygen saturation (SpO2) can be particularly critical, as respiratory depression is a known, albeit rare, risk associated with opioid analgesics. The integration of data from multiple biosensors can create a comprehensive physiological profile, allowing for a more nuanced understanding of how Tramadol impacts an individual’s vital signs over time.
Sleep Patterns and Activity Levels Analysis
Tramadol can also affect sleep architecture and overall activity levels. Patients may report insomnia, daytime somnolence, or changes in their daily routines. Wearable devices equipped with accelerometers and gyroscopes can track sleep duration, sleep stages (e.g., light, deep, REM sleep), and periods of wakefulness. Furthermore, they can monitor general physical activity throughout the day. By analyzing these patterns, researchers and clinicians can objectively assess the impact of Tramadol on sleep quality and daily functioning.
Changes in sleep patterns, such as fragmented sleep or increased periods of restlessness, could indicate that Tramadol is disrupting the natural sleep cycle. Similarly, significant reductions in overall daily activity, when not explained by the underlying condition being treated, might suggest fatigue or other central nervous system effects of the medication. The ability to correlate these objective activity and sleep data with Tramadol dosage and timing can provide valuable insights into its long-term effects on an individual’s well-being and functional capacity.
Pharmacogenomics and Personalized Medicine: Predicting Tramadol’s Response with Genetic Data
Individual responses to medications are significantly influenced by genetic makeup. Pharmacogenomics, the study of how genes affect a person’s response to drugs, is a rapidly advancing field that promises to revolutionize how medications like Tramadol are prescribed. By understanding an individual’s genetic profile, healthcare providers can potentially predict how effectively they will metabolize Tramadol and their likelihood of experiencing certain side effects.
Cytochrome P450 Enzymes and Tramadol Metabolism
Tramadol is primarily metabolized in the liver by cytochrome P450 (CYP) enzymes, most notably CYP2D6 and CYP3A4. Genetic variations in these enzymes can lead to significant differences in drug metabolism. For example, individuals with certain genetic variants of CYP2D6 are classified as poor metabolizers, intermediate metabolizers, extensive metabolizers, or ultra-rapid metabolizers. This classification directly impacts the conversion of Tramadol to its active metabolite, O-desmethyltramadol (M1), which is responsible for a substantial portion of its analgesic effect.
Poor metabolizers may not achieve adequate pain relief with standard doses of Tramadol because their bodies cannot efficiently convert it to the active M1 metabolite. Conversely, ultra-rapid metabolizers may convert Tramadol too quickly, leading to higher levels of M1 and an increased risk of opioid-related side effects, including potentially dangerous respiratory depression. Pharmacogenomic testing, which analyzes an individual’s CYP2D6 genotype, can inform dosage adjustments and guide the selection of alternative analgesics, thereby enhancing both efficacy and safety.
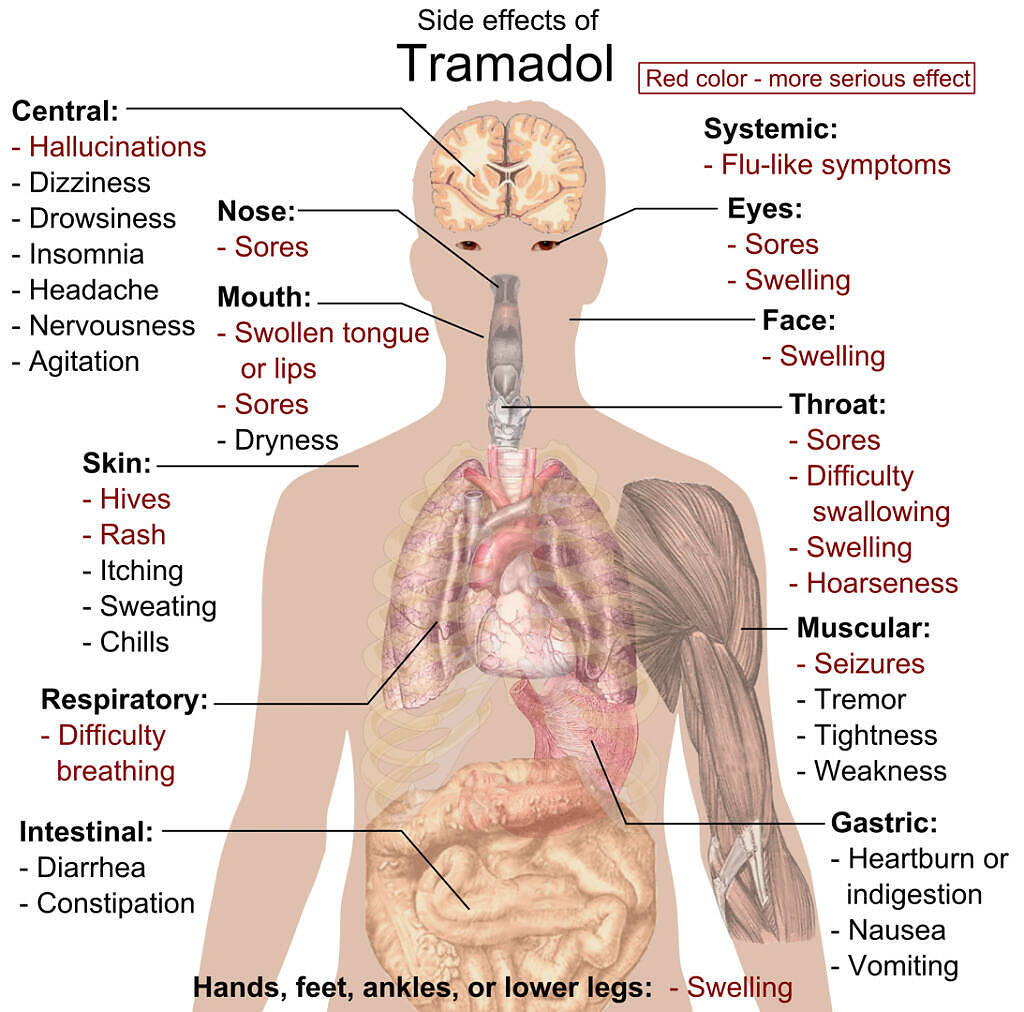
Serotonin Syndrome Risk Assessment
Another crucial aspect of Tramadol’s pharmacology is its effect on serotonin levels, due to its reuptake inhibition of norepinephrine and serotonin. This can lead to serotonin syndrome, a potentially life-threatening condition characterized by a cluster of symptoms including agitation, confusion, rapid heart rate, high blood pressure, dilated pupils, muscle rigidity, and heavy sweating. Certain genetic variants in genes involved in serotonin transport and metabolism, in conjunction with CYP2D6 variants, might predispose individuals to a higher risk of developing serotonin syndrome when taking Tramadol, especially if they are also on other serotonergic medications like SSRIs or SNRIs.
By analyzing an individual’s genetic predisposition for altered serotonin signaling pathways, alongside their CYP2D6 metabolizer status, healthcare providers can perform a more comprehensive risk assessment for serotonin syndrome. This personalized approach allows for proactive management, such as carefully monitoring patients with a higher genetic risk, adjusting dosages, or avoiding concurrent use of other serotonergic agents. The integration of pharmacogenomic data into clinical practice is moving towards a future where medication prescribing is less empirical and more precisely tailored to an individual’s unique biological blueprint, thereby answering the question of “what will Tramadol do to you” with an unprecedented level of personalization.
