Pulmonary edema, commonly referred to as “water in the lungs,” is a serious medical condition characterized by the abnormal accumulation of fluid in the air sacs (alveoli) of the lungs. This fluid buildup impairs gas exchange, making it difficult for the body to receive the oxygen it needs. While the physiological processes behind pulmonary edema are well-understood, the continuous and precise monitoring of its presence and progression has historically posed significant challenges. In recent years, however, technological innovation has begun to revolutionize how we approach the diagnosis, monitoring, and management of this critical condition. This article explores the cutting-edge technological advancements that are transforming our understanding and treatment of pulmonary edema.
The Evolving Landscape of Pulmonary Edema Detection
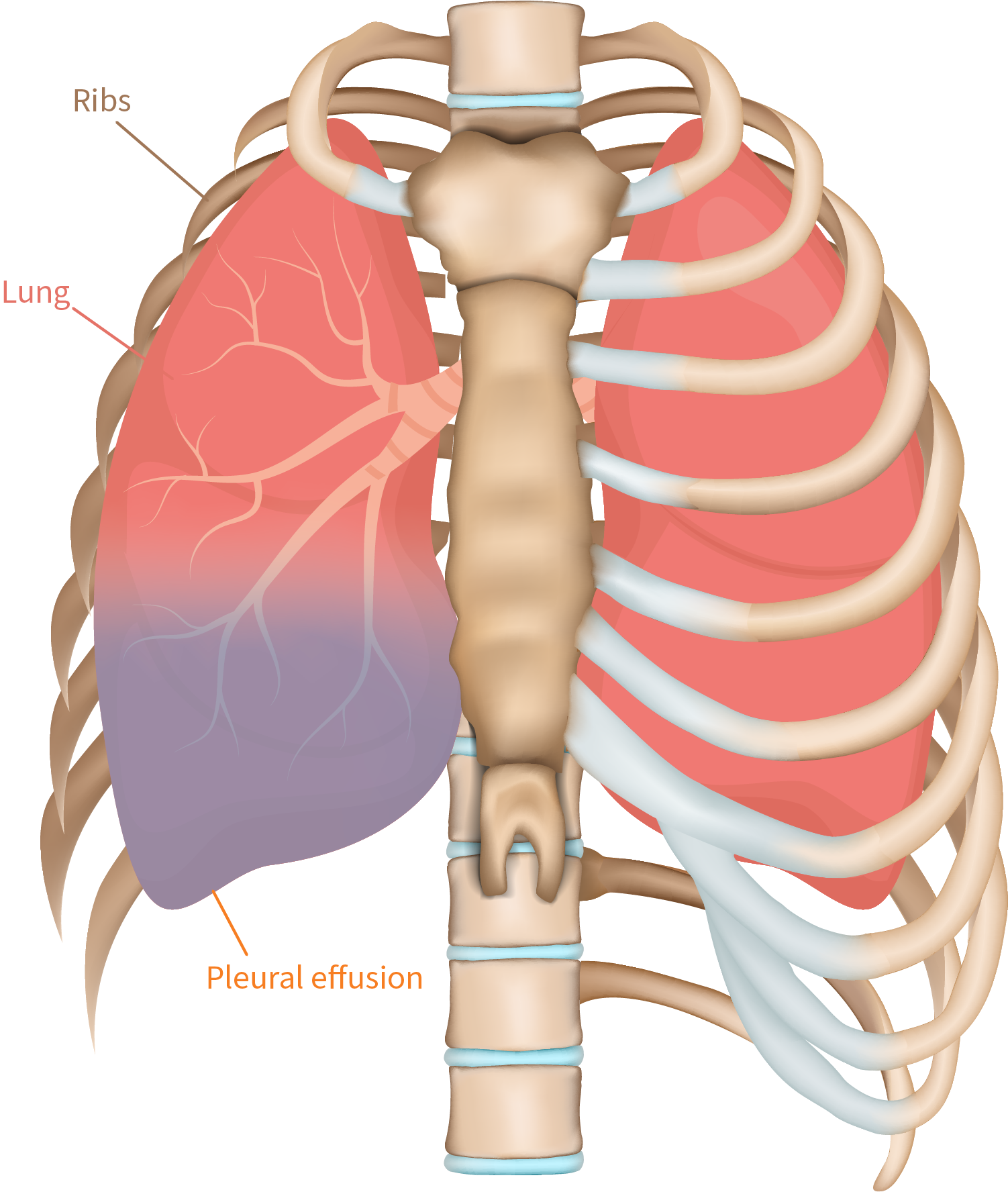
Traditionally, the diagnosis of pulmonary edema has relied on a combination of clinical symptoms, physical examination findings, and radiographic imaging. While effective, these methods often provide a snapshot in time and may not offer the continuous, granular data required for optimal patient management, especially in critical care settings. The push for earlier detection, more accurate quantification, and non-invasive monitoring has fueled a surge in technological innovation.
Early Warning Systems and Predictive Analytics
One of the most promising avenues of technological intervention lies in the development of early warning systems and predictive analytics. By integrating data from various physiological monitoring devices, advanced algorithms can identify subtle patterns and trends that may precede the overt manifestation of pulmonary edema.
Continuous Physiological Monitoring and Data Fusion
Modern intensive care units (ICUs) are equipped with a plethora of devices that continuously measure vital signs such as heart rate, blood pressure, oxygen saturation (SpO2), and respiratory rate. The true innovation comes from the ability to fuse this disparate data into a comprehensive picture. Artificial Intelligence (AI) and machine learning (ML) algorithms are being trained on vast datasets to recognize complex correlations that might elude human observation. For example, a slight but persistent increase in respiratory rate, coupled with subtle changes in heart rate variability and a dip in SpO2, could be an early indicator of impending fluid accumulation. These systems can then alert healthcare providers to potential issues before they become critical, allowing for proactive intervention.
Biomarker Detection and Biosensors
While not as widespread as vital sign monitoring, research is actively exploring the use of advanced biosensors for the detection of specific biomarkers associated with pulmonary edema. These could include inflammatory markers or indicators of cardiac strain. Miniature, implantable, or wearable biosensors could offer continuous monitoring of these markers, providing an even earlier warning signal than physiological parameters alone. The challenge here lies in developing sensors that are both accurate, reliable, and minimally invasive for long-term use.
Advanced Imaging Techniques and Computational Analysis
Imaging has always been a cornerstone in the diagnosis of pulmonary edema, with chest X-rays and CT scans providing visual evidence of fluid. However, technological advancements are making these imaging modalities more powerful and informative, moving beyond simple visualization to quantitative analysis.
High-Resolution Computed Tomography (HRCT) and Quantitative Analysis
While not a daily diagnostic tool due to radiation exposure, HRCT can provide highly detailed images of lung architecture. Advanced computational imaging techniques can then be applied to HRCT scans to precisely quantify the extent and distribution of interstitial and alveolar fluid. Algorithms can segment affected areas, measure fluid density, and track changes over time. This level of quantitative analysis offers a degree of precision that was previously unattainable, enabling clinicians to better assess the severity of pulmonary edema and the effectiveness of treatments.
Ultrasound in Respiratory Assessment
Point-of-care ultrasound (POCUS) has emerged as a revolutionary tool in various medical specialties, and its application in respiratory medicine is rapidly growing. Lung ultrasound can detect B-lines, which are vertical artifacts originating from the pleural line and extending down the lung parenchyma. The presence and number of these B-lines are highly indicative of interstitial fluid. Specialized ultrasound probes and advanced image processing algorithms are enhancing the sensitivity and specificity of lung ultrasound for detecting and quantifying pulmonary edema, even in its early stages. This non-invasive, radiation-free technique can be performed at the bedside, providing real-time information to guide clinical decisions.
Innovations in Monitoring and Management Technologies
Beyond diagnosis, technology is also playing a crucial role in the ongoing monitoring of patients with pulmonary edema and in guiding therapeutic interventions. The goal is to provide continuous, non-invasive, and actionable data to optimize patient care.
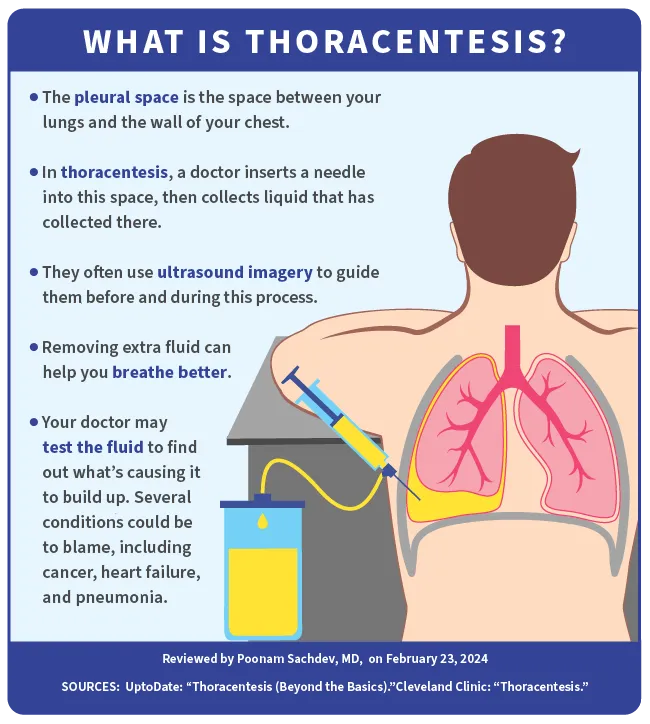
Non-Invasive Ventilation and Oxygen Delivery Systems
For patients experiencing significant respiratory distress due to pulmonary edema, ventilation support is often necessary. Technological advancements in non-invasive ventilation (NIV), such as bilevel positive airway pressure (BiPAP) and continuous positive airway pressure (CPAP) machines, have significantly improved patient comfort and outcomes. These devices deliver pressurized air through a mask, helping to keep the alveoli open and improve oxygenation without the need for endotracheal intubation. Smart NIV systems are also emerging, capable of automatically adjusting pressure levels based on real-time patient respiratory effort, thereby enhancing efficacy and reducing patient discomfort.
Smart Oxygen Delivery Devices
The delivery of supplemental oxygen is a critical component of managing pulmonary edema. “Smart” oxygen delivery systems are being developed that can dynamically adjust the flow rate of oxygen based on the patient’s actual oxygen saturation levels and respiratory patterns. This ensures that patients receive the precise amount of oxygen needed, avoiding both hypoxia and hyperoxia, both of which can have detrimental effects. These systems can also log data, providing valuable insights into the patient’s oxygenation trends over time.
Remote Monitoring and Telehealth Solutions
The COVID-19 pandemic accelerated the adoption of remote monitoring and telehealth, and these technologies hold immense promise for managing chronic conditions that can lead to or be exacerbated by pulmonary edema, such as heart failure.
Wearable Health Trackers and Remote Patient Monitoring Platforms
Wearable devices, ranging from sophisticated smartwatches to dedicated medical-grade sensors, can continuously collect data on vital signs, activity levels, and even subtle changes in body composition that might indicate fluid retention. This data can be transmitted wirelessly to secure cloud-based platforms, allowing healthcare providers to monitor patients remotely. If concerning trends are detected, such as a rapid weight gain or persistent elevated heart rate, the system can flag the patient for follow-up, potentially preventing hospitalizations.
Virtual Consultations and AI-Powered Health Assistants
Telehealth platforms facilitate virtual consultations between patients and their healthcare teams, reducing the need for in-person visits. Coupled with remote monitoring data, these consultations can be highly effective for managing conditions like heart failure. Furthermore, AI-powered health assistants or chatbots can provide patients with personalized advice, medication reminders, and guidance on symptom management, empowering them to play a more active role in their own care.
The Future: Integrated Systems and Personalized Medicine
The ultimate goal of technological innovation in the context of pulmonary edema is to move towards highly integrated systems that offer personalized and proactive care. This involves the seamless interplay of various technologies to provide a comprehensive and dynamic understanding of each patient’s condition.
Predictive Modeling for Individual Risk Stratification
By leveraging vast amounts of patient data, including genetic predispositions, lifestyle factors, and real-time physiological information, advanced AI models can be developed to stratify individuals based on their risk of developing pulmonary edema. This allows for targeted preventative strategies and earlier, more aggressive interventions for high-risk individuals. The concept of precision medicine is central here, tailoring diagnostic and therapeutic approaches to the unique biological and clinical profile of each patient.
Real-time Data Integration and Decision Support
Imagine a future where a patient’s wearable sensor data, bedside monitors, and imaging results are all fed into an AI-powered decision support system. This system could continuously analyze the integrated data, alert clinicians to subtle changes indicative of pulmonary edema, and even suggest optimal treatment adjustments in real-time. This level of integration has the potential to significantly improve the speed and accuracy of medical interventions, leading to better patient outcomes and potentially saving lives.
Nanotechnology and Novel Therapeutic Delivery
While still in early research phases, nanotechnology offers exciting possibilities for future advancements. Nanoparticles could be engineered to deliver therapeutic agents directly to the affected areas of the lungs, minimizing systemic side effects and maximizing treatment efficacy. Furthermore, nanosensors could offer unprecedented sensitivity for early detection of disease markers at the cellular level.
In conclusion, while “water in the lungs” is a medical term for a critical condition, the technological innovations driving its diagnosis, monitoring, and management are deeply rooted in the realm of Tech & Innovation. From AI-driven predictive analytics and advanced imaging to sophisticated non-invasive ventilation and remote monitoring platforms, technology is not only enhancing our understanding of pulmonary edema but also fundamentally transforming how we care for patients affected by it. The continuous evolution of these technologies promises a future where pulmonary edema can be detected earlier, managed more effectively, and ultimately, where patient outcomes are significantly improved.
