Pregnancy is a journey marked by profound physiological changes, preparing the female body for the monumental task of bringing new life into the world. Among these transformations, cervical dilation stands out as a critical indicator of labor’s progression. Understanding what dilation means, how it’s measured, and what influences it is essential for expectant parents and healthcare providers alike. This article delves into the intricacies of cervical dilation, exploring its significance throughout pregnancy and its role in childbirth.
The Cervix: A Gateway to Birth
The cervix, a cylindrical structure connecting the uterus to the vagina, plays a pivotal role in a healthy pregnancy and a successful labor. Throughout gestation, the cervix remains long, firm, and closed, acting as a protective barrier for the developing fetus. Its strength and integrity are paramount in preventing premature birth and supporting the growing weight of the baby.

Anatomy and Physiology of the Cervix
The cervix is primarily composed of strong connective tissues, including collagen and elastin, which provide its structural integrity. It also contains glands that produce mucus, forming a plug that seals the cervical canal. This “mucus plug” serves as a crucial defense against ascending infections, safeguarding the uterine environment. During pregnancy, hormonal influences, particularly progesterone, maintain the cervix in its closed, firm state, preventing any premature opening or effacement.
The Cervix’s Role in Maintaining Pregnancy
As pregnancy progresses, the cervix’s ability to remain closed and firm is vital. Any weakness or premature change in the cervix can lead to cervical insufficiency, a condition that can result in miscarriage or premature delivery. The cervix essentially acts as a “gatekeeper,” ensuring that the pregnancy continues to term without disruption. Its quiescent state is maintained by a complex interplay of hormones, mechanical pressure from the growing uterus, and local factors.
Cervical Dilation: The Beginning of Labor’s End
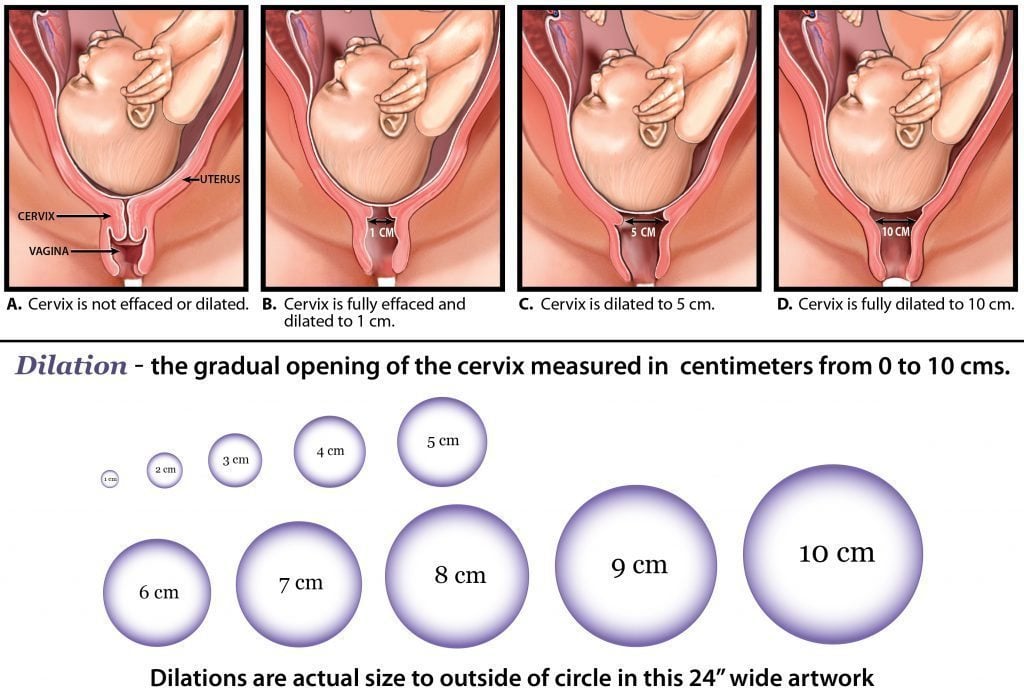
Cervical dilation refers to the widening of the opening of the cervix. This process is a cornerstone of labor, signifying the body’s preparation to expel the fetus. Dilation is measured in centimeters, ranging from 0 to 10.
Understanding the Dilation Scale: 0 to 10 Centimeters
The dilation scale is a standardized method used by healthcare professionals to track the progress of labor.
- 0 cm: The cervix is closed.
- 1-3 cm: This is considered early labor or the latent phase. The cervix begins to soften, thin out (efface), and open slightly. Contractions may be mild and irregular.
- 4-7 cm: This is active labor. Contractions become stronger, more frequent, and more regular. The cervix dilates more rapidly during this phase.
- 8-10 cm: This is transition, the most intense phase of labor. The cervix is nearly or fully dilated, and contractions are very strong.
- 10 cm: The cervix is fully dilated, and the mother is ready to push the baby out.
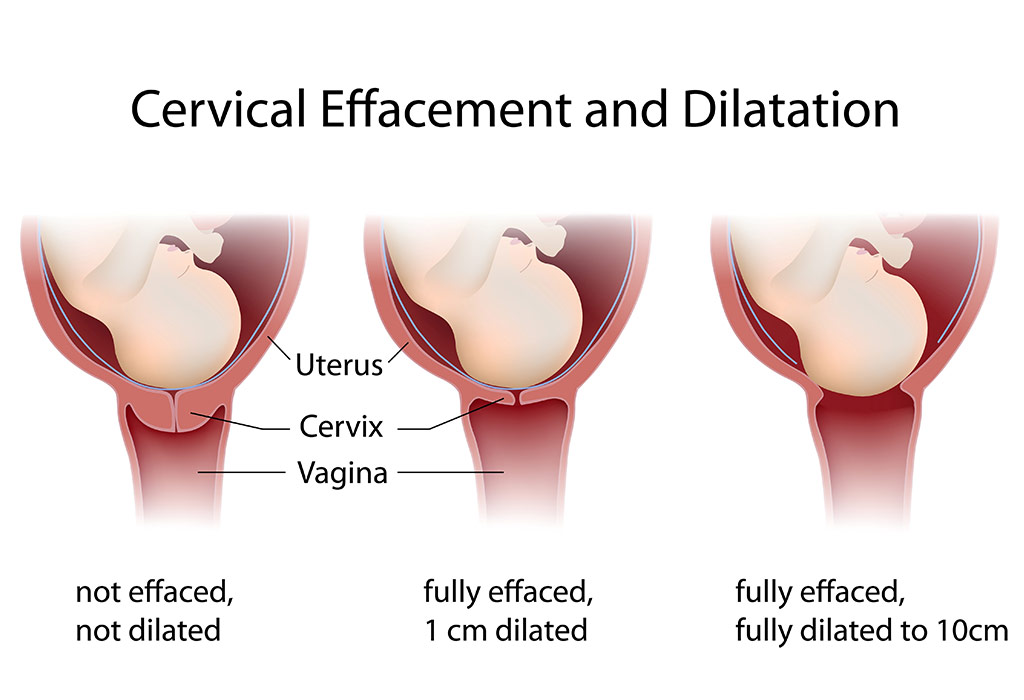
Effacement: The Cervix Thinning Out
Alongside dilation, effacement is another critical process that occurs during labor. Effacement refers to the thinning and shortening of the cervix. It is typically measured as a percentage, from 0% (fully long and thick) to 100% (completely thinned out). Dilation and effacement often occur simultaneously, with the cervix gradually opening and thinning in preparation for birth. For instance, a cervix might be described as “50% effaced and 3 cm dilated.”
How Dilation is Measured: The Digital Exam
Cervical dilation and effacement are primarily assessed through digital vaginal examinations performed by healthcare providers. By inserting gloved fingers into the vagina, a healthcare professional can feel the cervix and estimate its dilation and effacement. While this method is subjective and can vary slightly between examiners, it remains the standard clinical practice for monitoring labor progression. The frequency of these exams is determined by the stage of labor and the individual’s progress.
Factors Influencing Cervical Dilation
Several factors can influence the rate and pattern of cervical dilation. While the biological mechanisms are complex, certain elements are known to play a significant role.
The Role of Uterine Contractions
Uterine contractions are the primary driving force behind cervical dilation and effacement. As the powerful muscles of the uterus contract, they exert downward pressure on the cervix, gradually pulling it open and thinning it out. The intensity, frequency, and duration of these contractions directly impact the speed at which dilation occurs. Effective contractions are crucial for progressing labor, and sometimes medical interventions are needed to augment them.
Hormonal Changes and Labor Onset
Hormonal shifts play a crucial role in initiating and progressing labor, including cervical changes. Towards the end of pregnancy, the balance of hormones like estrogen, progesterone, prostaglandins, and oxytocin changes. Estrogen helps soften the cervix, making it more responsive to oxytocin, the hormone responsible for uterine contractions. Prostaglandins, in particular, are potent agents that can ripen and dilate the cervix, even before labor officially begins.
Previous Pregnancies and Births
A woman’s obstetric history can significantly influence cervical dilation.
- Multiparous women (those who have given birth before): Typically experience faster dilation and effacement in subsequent labors compared to first-time mothers (nulliparous women). This is because the cervix has already been stretched and may be more pliable.
- Parity: The number of previous vaginal births can affect labor patterns. However, each pregnancy and birth is unique, and individual variations are common.
Fetal Position and Presentation
The position and presentation of the baby in the uterus can also impact cervical dilation. Ideally, the baby presents head-down (cephalic presentation) and facing the mother’s back (occiput anterior position). This optimal presentation allows the baby’s head to apply even pressure to the cervix, facilitating dilation. Malpresentations, such as a breech (feet or buttocks first) or transverse (sideways) position, can sometimes slow down labor progression or necessitate different birth interventions.
Dilation Beyond Labor: Other Considerations
While cervical dilation is most prominently associated with labor and childbirth, there are other contexts in which the cervix may undergo changes in opening.
Cervical Ripening
Cervical ripening refers to the process of preparing the cervix for labor when it is not yet ready. This may be necessary for inductions of labor due to medical reasons, such as post-term pregnancy, preeclampsia, or fetal distress. Methods for cervical ripening include:
- Mechanical methods: Such as inserting a balloon catheter into the cervix to gradually stretch it.
- Medications: Like prostaglandins (gel or suppositories) or oxytocin (IV infusion) to stimulate contractions and cervical changes.
Cervical Insufficiency and Cerclage
Cervical insufficiency, also known as a weak cervix, is a condition where the cervix begins to open and thin out prematurely, typically in the second trimester of pregnancy, without labor contractions. This can lead to miscarriage or preterm birth. To address cervical insufficiency, a procedure called a cervical cerclage may be performed. This involves stitching the cervix closed to prevent it from dilating and effacing too early. The stitch is usually removed before labor begins or when labor is established.
Postpartum Dilation
While the primary focus is on dilation during labor, some degree of cervical opening may persist for a short period postpartum. The cervix will gradually close over the days and weeks following birth, returning to its non-pregnant state. However, the rate of closure can vary among individuals.
Conclusion: A Vital Indicator of Birth
Cervical dilation is a fundamental aspect of labor and delivery, providing healthcare providers with a crucial measure of a pregnancy’s progression. From the initial subtle changes in early labor to the full dilation of 10 centimeters, each stage signifies a step closer to welcoming a new life. Understanding the factors that influence dilation, the methods of measurement, and its implications beyond active labor empowers expectant parents and highlights the remarkable adaptability of the female body in its journey through pregnancy and childbirth.
