Understanding the optimal timing for conception is a critical piece of knowledge for individuals and couples aiming to start or expand their families. While the biological process of conception might seem straightforward, human fertility operates within a dynamic cycle, influenced by a variety of factors that peak at specific times. This article delves into the science and practicalities of identifying the “best time for conception,” focusing on the female menstrual cycle and its implications for maximizing the chances of a successful pregnancy.
The Crucial Role of the Menstrual Cycle
The female reproductive system is designed to facilitate conception by releasing an egg (ovulation) during a specific window each month. The menstrual cycle, a complex interplay of hormones, dictates this process. Successfully conceiving relies on having intercourse during this fertile window, which includes the days leading up to ovulation and the day of ovulation itself.
Understanding Ovulation: The Heart of Fertility
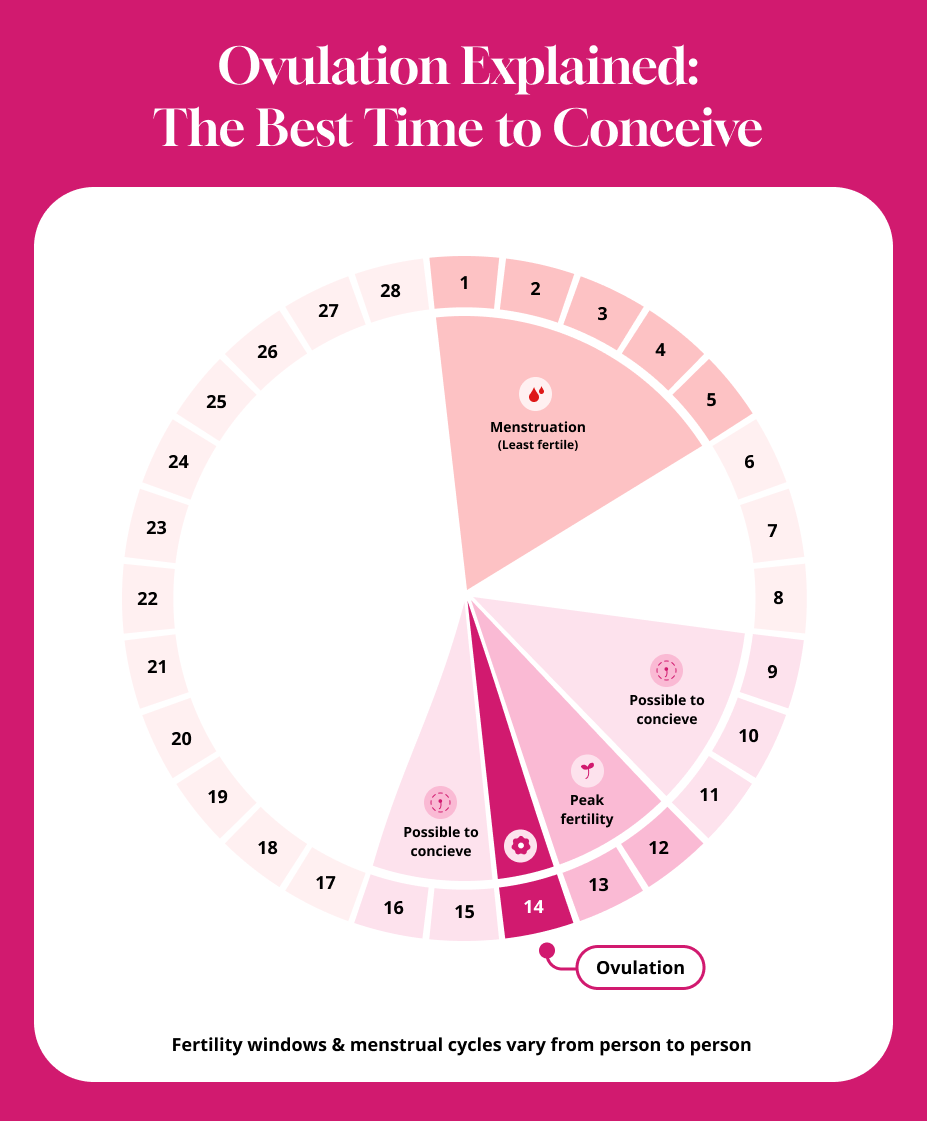
Ovulation is the monthly release of a mature egg from one of the ovaries. This egg then travels down the fallopian tube, where it can be fertilized by sperm. The egg is viable for approximately 12 to 24 hours after ovulation. However, sperm can survive in the female reproductive tract for up to five days. This means that intercourse occurring several days before ovulation can still lead to conception, as the sperm can remain viable and fertilize the egg once it’s released.
Key Stages of the Menstrual Cycle:
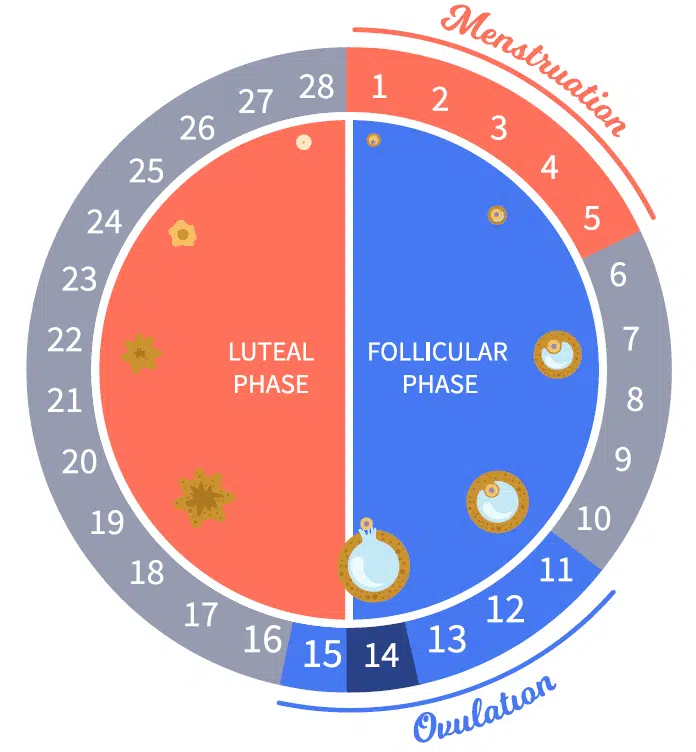
- Menstruation (Days 1-5 approximately): This is the shedding of the uterine lining, characterized by bleeding. While conception is highly unlikely during menstruation, it marks the beginning of a new cycle.
- Follicular Phase (Days 1-14 approximately): This phase begins on the first day of menstruation and ends with ovulation. During this time, follicles in the ovaries mature, and one dominant follicle containing an egg develops. The uterine lining also begins to thicken in preparation for a potential pregnancy. Hormone levels, particularly estrogen, rise steadily.
- Ovulation (Mid-cycle, around Day 14 in a 28-day cycle): This is the release of the mature egg from the dominant follicle. This is the most fertile period. A surge in luteinizing hormone (LH) triggers ovulation.
- Luteal Phase (Days 14-28 approximately): After ovulation, the ruptured follicle transforms into the corpus luteum, which produces progesterone. Progesterone prepares the uterine lining for implantation. If fertilization and implantation occur, the corpus luteum continues to produce hormones. If not, it degenerates, leading to a drop in hormone levels and the onset of menstruation.
The Fertile Window: When Conception is Most Likely
The “fertile window” encompasses the days in a woman’s cycle when pregnancy is possible. This window is not limited to the day of ovulation. Given the lifespan of sperm (up to five days) and the egg (12-24 hours), the fertile window typically begins about five days before ovulation and extends through the day of ovulation.
- The Day of Ovulation: This is the most fertile day.
- The 4-5 Days Preceding Ovulation: Intercourse during these days has a high probability of leading to conception because sperm can survive and await the egg’s release.
- The Day After Ovulation: There is a small chance of conception on this day, as the egg is still viable for a short period.
Therefore, the optimal time to have intercourse to conceive is within this fertile window, particularly in the days leading up to and including ovulation.
Methods for Identifying Your Fertile Window
Pinpointing ovulation accurately is key to maximizing your chances of conception. Several methods can help you identify your fertile window, ranging from simple observation to more technologically advanced tracking.
Tracking Basal Body Temperature (BBT)
Basal Body Temperature (BBT) refers to your resting body temperature taken first thing in the morning before getting out of bed. After ovulation, progesterone levels rise, causing a slight increase in BBT, typically by 0.5 to 1 degree Fahrenheit (0.3 to 0.6 degrees Celsius).
- How to Track: Using a specialized BBT thermometer, take your temperature every morning at the same time, before any activity. Record the readings on a chart or in an app.
- Interpreting the Data: A sustained rise in BBT for at least three consecutive days indicates that ovulation has likely occurred. While this method confirms ovulation after it has happened, it’s useful for identifying patterns over several cycles. By tracking BBTs over time, you can begin to predict when ovulation might occur in future cycles.
- Limitations: BBT can be affected by factors like illness, alcohol consumption, stress, and poor sleep. It is not a real-time predictor of ovulation but rather a retrospective confirmation.
Monitoring Cervical Mucus Changes
Cervical mucus is a natural fluid produced by the cervix. Its consistency and appearance change throughout the menstrual cycle in response to hormonal fluctuations. These changes can provide valuable clues about your fertility.
- Stages of Cervical Mucus:
- Dry or Sticky: Usually present during less fertile days.
- Creamy or Cloudy: Indicates increasing fertility.
- Watery: High fertility.
- Raw Egg White Consistency (Stretchy and Clear): This is the most fertile type of cervical mucus, often referred to as “egg white cervical mucus” (EWCM). It appears a day or two before ovulation and signifies that ovulation is imminent.
- How to Track: Regularly observe the mucus from your vaginal opening using toilet paper or by inserting a clean finger. Note its color, consistency, and whether it feels wet, dry, or slippery.
- Interpreting the Data: The appearance of EWCM is a strong indicator that you are entering your fertile window. Having intercourse when you observe this type of mucus significantly increases your chances of conception.
Utilizing Ovulation Predictor Kits (OPKs)
Ovulation Predictor Kits (OPKs) are over-the-counter urine tests that detect the surge in luteinizing hormone (LH) that occurs 24 to 36 hours before ovulation.
- How to Use: Typically, you start testing a few days before you expect to ovulate. You urinate on a test strip. A positive result, indicated by two lines (one control line and one test line of similar or darker intensity), signals that you are likely to ovulate soon.
- Interpreting the Data: A positive OPK indicates that ovulation is approaching, making it an excellent time for intercourse. It’s important to follow the kit’s instructions regarding the best time of day to test and how many days to test to ensure accuracy.
- Advantages: OPKs are convenient and provide a more direct indication of imminent ovulation compared to BBT charting.
Understanding Calendar Methods and Cycle Apps
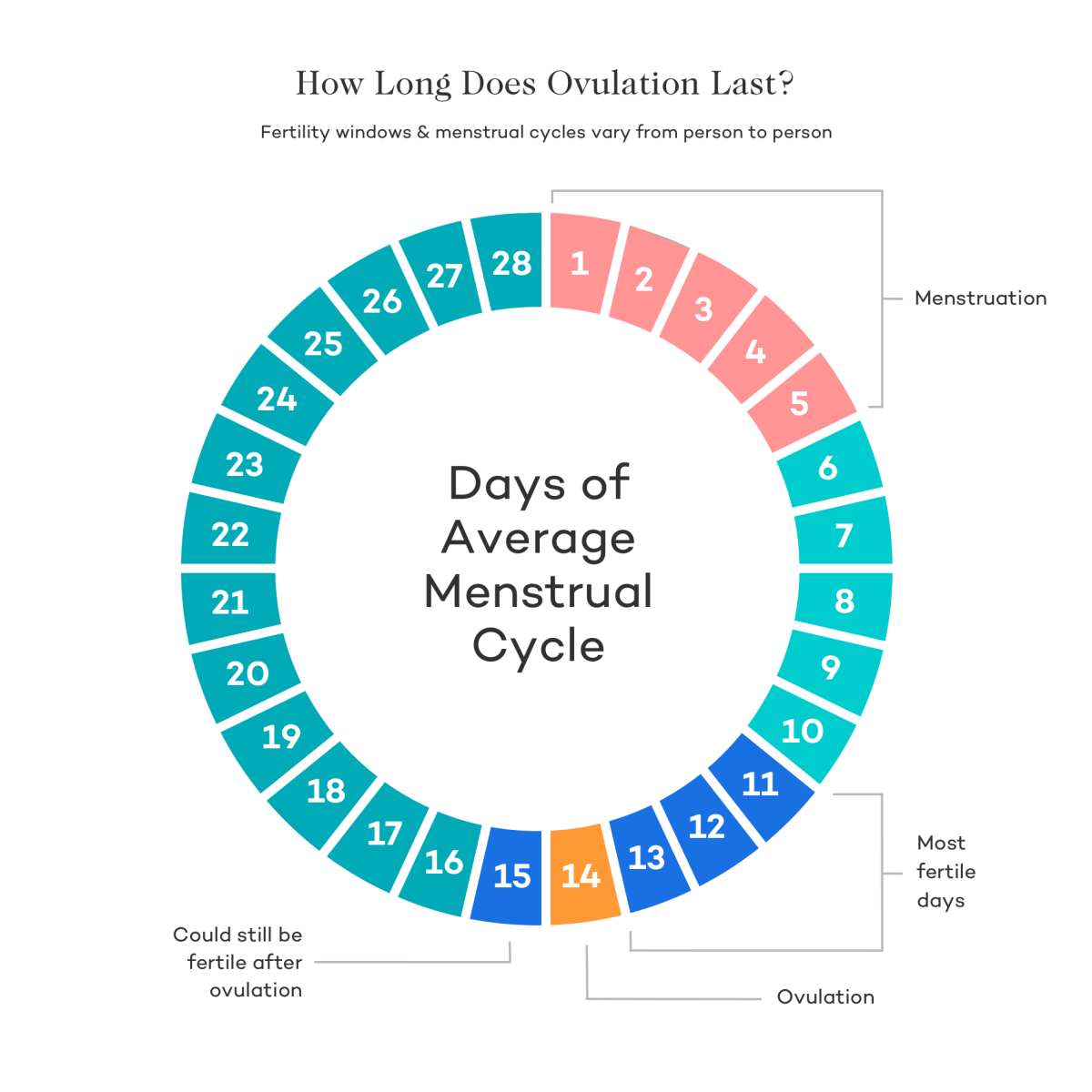
The calendar method involves calculating your fertile window based on the length of your previous menstrual cycles. For women with regular cycles, this can provide a general estimate.
- How to Calculate: Subtract 18 days from the start of your shortest cycle to estimate the beginning of your fertile window, and subtract 11 days from the start of your longest cycle to estimate the end of your fertile window.
- Cycle Tracking Apps: Many smartphone applications can help you track your menstrual cycle, BBT, cervical mucus, and OPK results. These apps often analyze your data to predict your fertile window and ovulation day, offering a consolidated view of your fertility signs.
- Limitations: The calendar method is less reliable for women with irregular cycles, as cycle lengths can vary significantly. While apps can be helpful tools, they are most effective when combined with other tracking methods.
Lifestyle Factors and Maximizing Conception Chances
Beyond identifying the fertile window, several lifestyle factors can positively influence fertility and the chances of a successful conception. Both partners play a role, and adopting healthy habits can create an optimal environment for conception.
Nutrition and Weight Management
A balanced diet rich in fruits, vegetables, whole grains, and lean proteins provides essential nutrients for reproductive health.
- Key Nutrients for Fertility:
- Folic Acid (Folate): Crucial for preventing neural tube defects in the developing fetus, folic acid supplementation is recommended for women trying to conceive.
- Iron: Supports healthy ovulation and red blood cell production.
- Omega-3 Fatty Acids: Found in fatty fish, flaxseeds, and walnuts, they play a role in hormone regulation.
- Antioxidants: Found in berries, nuts, and dark leafy greens, antioxidants help protect reproductive cells from damage.
- Weight Management: Being underweight or overweight can disrupt hormonal balance and affect ovulation. Aiming for a healthy Body Mass Index (BMI) is beneficial for both men and women trying to conceive. For women, being significantly underweight can lead to irregular or absent ovulation, while being overweight or obese can affect egg quality and increase the risk of pregnancy complications.
The Impact of Exercise
Moderate exercise can be beneficial for fertility, promoting healthy weight and reducing stress. However, excessive or strenuous exercise can sometimes negatively impact reproductive health, particularly in women.
- Benefits of Moderate Exercise: Regular physical activity can improve circulation, reduce stress hormones, and contribute to overall well-being.
- Risks of Over-Exercise: For women, very intense or prolonged exercise can lead to hormonal imbalances that disrupt ovulation and menstrual cycles. It’s advisable to maintain a moderate exercise routine and consult with a healthcare provider if you have concerns.
Stress Management and Sleep
Chronic stress can interfere with the hormones that regulate the reproductive system, potentially impacting ovulation and sperm production.
- Stress Reduction Techniques: Practices like yoga, meditation, deep breathing exercises, spending time in nature, and engaging in enjoyable hobbies can help manage stress levels.
- Importance of Sleep: Adequate sleep (7-9 hours per night) is crucial for hormone regulation and overall health. Poor sleep can exacerbate stress and negatively affect fertility.
Avoiding Harmful Substances
Certain substances can adversely affect fertility in both men and women.
- Smoking: Damages eggs and sperm, reducing fertility and increasing the risk of miscarriage and birth defects. Quitting smoking is one of the most significant steps a couple can take to improve their chances of conception.
- Excessive Alcohol Consumption: Can disrupt menstrual cycles in women and lower sperm count and quality in men. Moderation or avoidance is recommended when trying to conceive.
- Recreational Drugs: Can have severe negative impacts on fertility and fetal development.
- Caffeine: While moderate caffeine intake is generally considered safe, excessive consumption might be linked to reduced fertility. It’s advisable to limit intake.
When to Seek Professional Advice
While many couples conceive with regular, well-timed intercourse, sometimes professional guidance is necessary.
Understanding Fertility Concerns
Fertility is generally defined as the ability to conceive after one year of regular, unprotected intercourse. For women over 35, this timeframe is reduced to six months, as fertility naturally declines with age.
- Factors Affecting Fertility: A variety of factors can impact fertility in both men and women, including:
- Female Factors: Ovulatory disorders (e.g., PCOS), fallopian tube blockage, endometriosis, uterine abnormalities, and age-related decline in egg quality.
- Male Factors: Low sperm count, poor sperm motility, abnormal sperm morphology, and blockages in the reproductive tract.
- Unexplained Infertility: In some cases, no specific cause for infertility can be identified.
Consulting with a Healthcare Provider
If you have been trying to conceive for a significant period without success, or if you have any underlying health conditions that might affect fertility, it is advisable to consult with a healthcare provider or a fertility specialist.
- Initial Assessment: A healthcare provider can perform a thorough medical history review, conduct physical examinations, and recommend initial fertility tests. These may include hormone level assessments, ovulation monitoring, and semen analysis.
- Personalized Guidance: Based on your individual circumstances, a specialist can offer personalized advice, treatment options, and support throughout your fertility journey. Early intervention can often lead to more successful outcomes.
In conclusion, understanding the best time for conception involves a comprehensive approach that integrates knowledge of the menstrual cycle, accurate fertility tracking, and the adoption of healthy lifestyle practices. By proactively identifying your fertile window and making informed choices about your health, you can significantly enhance your chances of a successful pregnancy.
