The experience of a sore inside the mouth is a common, albeit uncomfortable, one. Whether it’s a sharp twinge when eating or a persistent ache, these oral lesions can significantly impact daily life. Understanding what these sores are called and their potential causes is the first step towards finding relief. This article delves into the various types of sores that can manifest within the oral cavity, exploring their characteristics, common triggers, and when to seek professional advice.
Understanding the Spectrum of Oral Sores
The term “sore inside your mouth” is a broad description. In medical and dental contexts, these lesions are often referred to by more specific names, depending on their appearance, location, and underlying cause. Broadly, they can be classified into two main categories: infectious and non-infectious.

Common Non-Infectious Oral Lesions
Many common mouth sores are not caused by bacteria or viruses, but rather by minor trauma, nutritional deficiencies, stress, or other systemic factors. These are often the most frequently encountered types of oral lesions.
Aphthous Ulcers (Canker Sores)
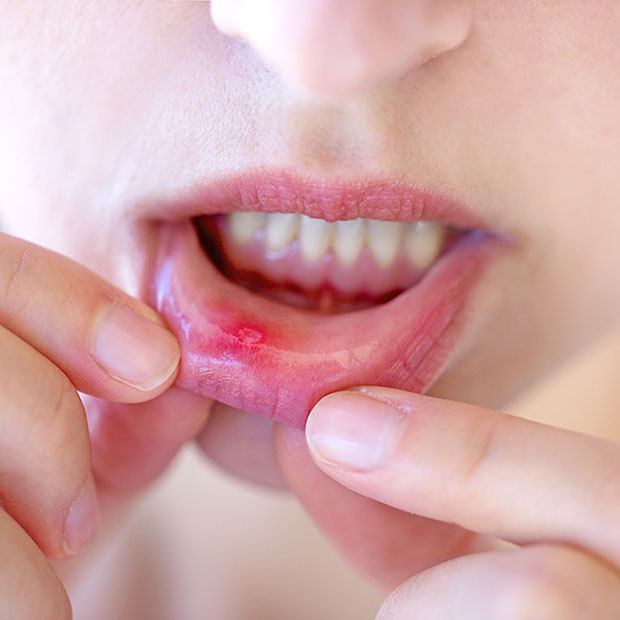
Perhaps the most common culprit for a “sore inside your mouth” is an aphthous ulcer, more colloquially known as a canker sore. These are small, shallow, painful lesions that appear on the soft tissues inside the mouth, such as the inside of the lips, cheeks, tongue, and the base of the gums.
- Appearance: Aphthous ulcers are typically round or oval with a white or yellowish center and a red border. They are not open wounds in the traditional sense but rather ulcerated areas of the mucous membrane.
- Symptoms: The primary symptom is pain, which can be mild to severe and is often exacerbated by eating, drinking, or talking. They can also cause a burning or tingling sensation before they become fully visible.
- Causes: The exact cause of canker sores is not fully understood, but several factors are believed to contribute to their development. These include:
- Minor Injury: Accidental biting of the cheek or tongue, irritation from dental appliances like braces or dentures, or even vigorous tooth brushing can trigger an outbreak.
- Stress and Fatigue: Emotional stress and lack of sleep are commonly reported triggers.
- Nutritional Deficiencies: Low levels of certain vitamins and minerals, particularly B vitamins (like B12), iron, and folic acid, have been linked to recurrent canker sores.
- Hormonal Changes: Some women experience canker sores around their menstrual cycle due to fluctuations in hormone levels.
- Allergies and Sensitivities: Certain foods, such as acidic fruits, chocolate, coffee, and nuts, can trigger canker sores in susceptible individuals. Sodium lauryl sulfate (SLS), an ingredient found in many toothpastes and mouthwashes, has also been implicated.
- Underlying Medical Conditions: While less common, canker sores can sometimes be a symptom of more serious conditions like celiac disease, inflammatory bowel disease (Crohn’s disease, ulcerative colitis), or a compromised immune system.
- Types of Aphthous Ulcers:
- Minor Aphthous Ulcers: These are the most common, typically measuring less than 1 centimeter in diameter and healing within 7-14 days without scarring.
- Major Aphthous Ulcers: These are larger, deeper, and more painful. They can measure over 1 centimeter and may take several weeks to heal, often leaving behind scars.
- Herpetiform Ulcers: These are characterized by multiple small sores that appear in clusters, resembling herpes simplex (cold sores), though they are not related to the herpes virus. They can be very painful and may take up to two weeks to heal.
Traumatic Ulcers
These are direct results of physical injury to the oral tissues. They are typically superficial and heal relatively quickly once the source of trauma is removed.
- Causes: As mentioned earlier, common causes include:
- Accidental biting of the cheek, lip, or tongue.
- Irritation from sharp edges of broken teeth or ill-fitting dental prosthetics.
- Burns from hot food or drinks.
- Aggressive tooth brushing or flossing.
- Irritation from certain foods or dental materials.
- Appearance: Traumatic ulcers are often irregular in shape and their appearance can vary depending on the nature of the injury. They are usually painful and may be accompanied by mild swelling or redness around the affected area.
Irritation Fibromas
While not strictly a “sore” in the sense of an ulceration, irritation fibromas are benign growths that can occur inside the mouth, often in response to chronic friction or irritation. They are firm lumps that can sometimes be mistaken for sores.
- Causes: Constant rubbing from teeth, dentures, or cheek biting can lead to the formation of these fibrous tissue overgrowths.
- Appearance: Fibromas are typically smooth, pink, and sessile (attached to the underlying tissue by a broad base) or pedunculated (attached by a stalk). They are usually painless unless they become irritated or inflamed.
Infectious Oral Lesions
Unlike non-infectious sores, these are caused by pathogens such as viruses, bacteria, or fungi. They often present with additional symptoms beyond localized pain.
Viral Infections
Certain viruses can cause sores inside the mouth. The most well-known is herpes simplex virus.
- Herpes Simplex Virus (HSV) – Oral Herpes:
- Primary Herpetic Gingivostomatitis: This is often the initial infection with HSV and typically occurs in children. It causes widespread inflammation of the gums (gingivitis) and multiple painful sores on the inside of the lips, cheeks, tongue, and palate. Symptoms can include fever, swollen lymph nodes, and general malaise.
- Recurrent Herpes Labialis (Cold Sores/Fever Blisters): While these usually appear on the outside of the lips, they can sometimes manifest as sores inside the mouth, particularly on the hard palate or gums. They often start as a tingling or burning sensation, followed by the development of small blisters that eventually break open, crust over, and heal.
- Hand, Foot, and Mouth Disease (HFMD): This is a common viral illness, usually affecting young children, caused by coxsackieviruses. It causes painful sores in the mouth, often on the tongue, gums, and inside of the cheeks, as well as a rash on the hands and feet.
Fungal Infections
Fungal infections, particularly Candida albicans, can lead to a common oral condition known as thrush.
- Oral Candidiasis (Thrush):
- Appearance: Thrush is characterized by creamy white patches that can be scraped off, revealing red, inflamed tissue underneath. These patches can appear on the tongue, inner cheeks, roof of the mouth, and throat.
- Symptoms: Sores or patches can be painful and may cause a burning sensation or a loss of taste.
- Causes: Thrush is more common in infants, the elderly, individuals with weakened immune systems (due to conditions like HIV/AIDS, cancer treatment, or immunosuppressant medications), and those using inhaled corticosteroids or wearing dentures. Antibiotic use can also disrupt the natural balance of microorganisms in the mouth, leading to an overgrowth of Candida.
Bacterial Infections
While less common as primary causes of widespread oral sores, certain bacterial infections can lead to localized lesions.
- Vincent’s Angina (Trench Mouth): This is a painful bacterial infection of the gums and mouth, characterized by inflammation, ulceration, and a foul-smelling breath. It’s often associated with poor oral hygiene, stress, and smoking. The sores are typically grayish-white and painful, with bleeding gums.
Less Common but Significant Causes
Beyond the everyday canker sores and minor irritations, certain systemic conditions or more serious oral pathology can present as mouth sores.
Oral Lichen Planus
Oral lichen planus is a chronic inflammatory condition that can affect the skin and mucous membranes. When it affects the mouth, it can manifest in various ways, including sores.
- Appearance: Oral lichen planus can appear as white, lacy lines (Wickham’s striae), red and swollen areas, or open sores (erosive lichen planus). The erosive form is often painful and can occur on the tongue, cheeks, or gums.
- Causes: The exact cause is unknown but is thought to be an immune-mediated condition. It can sometimes be triggered by certain medications or viral infections.
Autoimmune Diseases
Some autoimmune diseases, where the body’s immune system mistakenly attacks its own tissues, can cause oral sores.
- Behçet’s Disease: This is a rare disorder that causes inflammation in blood vessels throughout the body. It is characterized by recurrent oral ulcers, genital ulcers, eye inflammation, and skin lesions. The oral ulcers are often similar to canker sores but can be more severe and recurrent.
- Pemphigus Vulgaris: This is a rare autoimmune disease that causes blistering and sores on the skin and mucous membranes, including the mouth. The oral sores can be very painful and can precede skin lesions.
Oral Cancer
While the vast majority of mouth sores are benign, it is crucial to be aware that a persistent, non-healing sore or lump in the mouth could be a sign of oral cancer.
- Warning Signs: Any sore inside the mouth that does not heal within two to three weeks, or that bleeds easily, is red or white, or causes numbness, should be evaluated by a dental or medical professional. Other symptoms can include a lump or thickening in the cheek, difficulty chewing or swallowing, and changes in voice.

When to Seek Professional Help
While many oral sores are self-limiting and resolve on their own with home care, there are instances where professional medical or dental advice is necessary.
- Persistent Sores: If a sore inside your mouth does not heal within two to three weeks, it is essential to consult a dentist or doctor.
- Recurrent or Severe Sores: If you experience frequent or particularly painful canker sores, your healthcare provider can investigate potential underlying causes and recommend appropriate management strategies.
- Associated Symptoms: If mouth sores are accompanied by other symptoms such as fever, difficulty swallowing, a widespread rash, or swollen lymph nodes, seek medical attention promptly.
- Concerns about Oral Cancer: Any unusual or concerning changes in your mouth should be professionally evaluated.
In conclusion, the seemingly simple “sore inside your mouth” can have a variety of names and causes, ranging from minor irritations to indicators of systemic health issues. By understanding the different types of oral lesions and their potential origins, individuals can better manage their oral health and know when to seek expert guidance.
