The electrocardiogram (ECG), a cornerstone of modern cardiology, offers a non-invasive window into the heart’s electrical symphony. While the entire waveform provides a wealth of diagnostic information, the T-wave, specifically, represents a critical phase of this electrical cycle. In the realm of tech and innovation, understanding the T-wave is not merely about deciphering a biological signal; it’s about appreciating the sophisticated technology that captures, processes, and interprets these subtle electrical fluctuations to provide invaluable insights into cardiac health. This article delves into the technological underpinnings of ECG, focusing on the significance and interpretation of T-waves within the broader context of health monitoring innovation.
The Foundation of Cardiac Electrical Monitoring: ECG Technology and its Innovations
At its core, ECG technology is a marvel of bio-sensing and signal processing. It relies on the principle that the heart’s electrical activity, generated by the depolarization and repolarization of cardiac muscle cells, creates electrical currents that can be detected on the surface of the body. The evolution of ECG devices, from bulky analog machines to sophisticated digital systems integrated into wearable technology, exemplifies the rapid pace of innovation in health monitoring.
Principles of Electrical Signal Detection
The generation of an ECG signal begins with the ion flux across the membranes of cardiac myocytes. During depolarization, positive ions like sodium (Na+) and calcium (Ca2+) rush into the cell, creating a positive charge within the cell and a negative charge on the outer surface. This electrical event propagates through the myocardium, generating a measurable electrical field. Conversely, repolarization, the return of the cell to its resting negative charge, involves the outward movement of potassium ions (K+). The ECG machine, equipped with electrodes placed strategically on the skin, acts as a sensitive voltmeter, detecting these minute voltage differences that arise from the collective electrical activity of millions of heart cells. The arrangement and number of electrodes vary, with standard 12-lead ECGs employing 10 electrodes to provide a comprehensive, multi-dimensional view of the heart’s electrical field.
The Evolution of ECG Hardware and Software
Early ECG devices were analog, producing paper tracings that required manual interpretation by skilled clinicians. The advent of digital signal processing revolutionized ECG analysis. Digital ECG machines digitize the analog signals, allowing for amplification, filtering, and noise reduction through sophisticated algorithms. This has led to increased accuracy and consistency in readings. Furthermore, the miniaturization of electronic components has enabled the development of portable and even wearable ECG devices, such as smartwatches and patches. These innovations democratize cardiac monitoring, allowing for continuous or on-demand data collection outside of traditional clinical settings. The software powering these devices has also become increasingly intelligent, incorporating machine learning and artificial intelligence to assist in the automated detection of arrhythmias, ischemia, and other abnormalities, thereby augmenting the diagnostic capabilities of healthcare professionals.
Decoding the ECG Waveform: The T-Wave and its Technological Interpretation
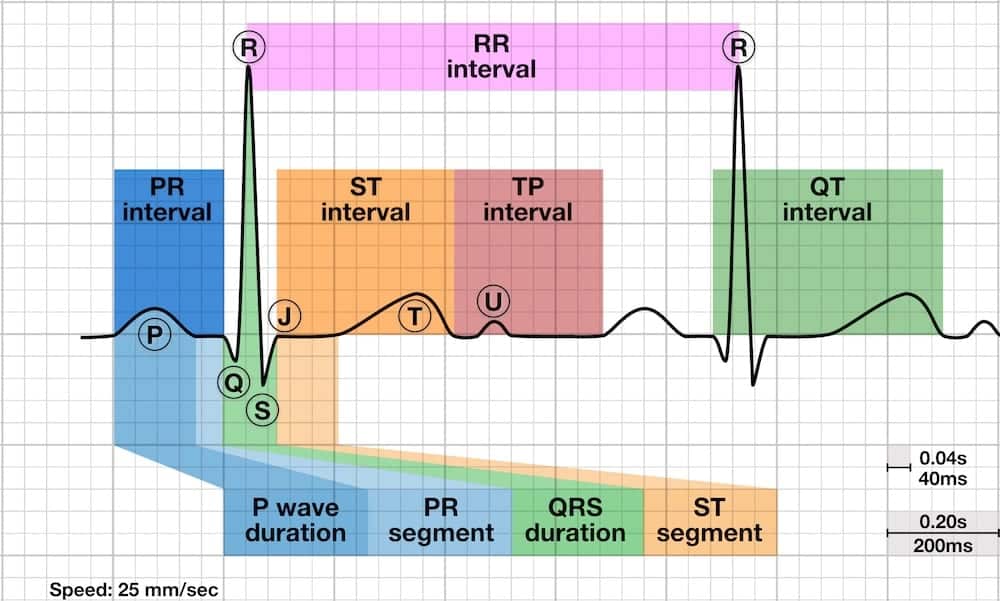
The ECG waveform is a graphical representation of the heart’s electrical cycle, composed of distinct waves and intervals, each corresponding to a specific electrical event. The P-wave represents atrial depolarization, the QRS complex signifies ventricular depolarization, and the T-wave marks the crucial phase of ventricular repolarization. Understanding the T-wave’s technological interpretation is key to appreciating its diagnostic value.
Ventricular Repolarization: The Electrical Reset
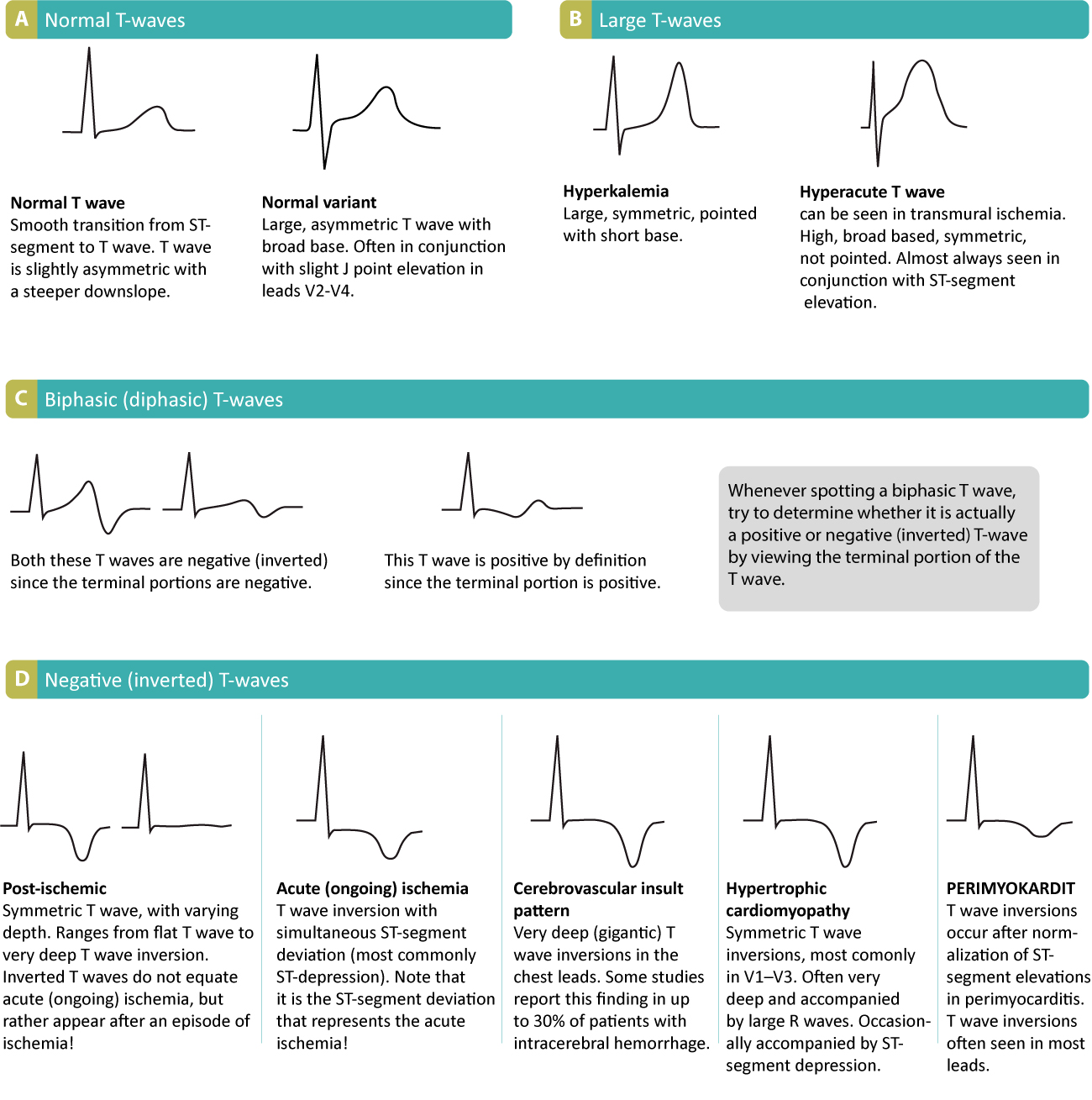
The T-wave on an ECG represents the repolarization of the ventricles, the heart’s main pumping chambers. Following the powerful electrical stimulus that causes the ventricles to contract (depolarization, represented by the QRS complex), the cardiac muscle cells must electrically reset themselves to be ready for the next beat. This process of repolarization is not uniform across the entire ventricular wall, which contributes to the T-wave’s typically rounded, asymmetric shape. The electrical potential changes during repolarization are detected by the ECG electrodes and translated into the characteristic upward deflection of the T-wave, which generally follows the QRS complex. The duration, amplitude, and morphology of the T-wave are meticulously analyzed by both human interpreters and sophisticated ECG analysis software.
Technological Analysis of T-Wave Morphology and Significance
Modern ECG interpretation increasingly relies on advanced algorithms to analyze T-wave characteristics. These algorithms can quantify T-wave amplitude, duration, and symmetry, and compare these parameters against established normative ranges. Deviations from the norm can indicate a range of cardiac conditions. For instance, flattened or inverted T-waves can be indicative of ischemia (reduced blood flow to the heart muscle) or electrolyte imbalances. Peaked T-waves can suggest hyperkalemia (high potassium levels), a potentially life-threatening condition. Furthermore, sophisticated algorithms can detect subtle changes in T-wave morphology that might be missed by the naked eye, such as T-wave alternans, which are beat-to-beat variations in T-wave shape that have been linked to an increased risk of sudden cardiac death. The integration of AI into ECG analysis is further enhancing this capability, enabling the detection of complex patterns and predictive markers of cardiac events.
Advanced Applications and Future Directions in ECG Technology
The continuous innovation in ECG technology extends beyond basic waveform analysis. The development of sophisticated signal processing techniques, coupled with the integration of artificial intelligence, is paving the way for more personalized and predictive cardiac care.
Wearable ECGs and Continuous Cardiac Monitoring
The proliferation of wearable devices has been a significant technological leap in cardiac monitoring. Smartwatches and fitness trackers equipped with ECG sensors allow for continuous or on-demand monitoring of heart rhythm and electrical activity. This enables early detection of arrhythmias like atrial fibrillation, a common condition that significantly increases stroke risk. The data collected by these devices can be wirelessly transmitted to healthcare providers, facilitating proactive management and timely intervention. The challenge here lies in ensuring the accuracy and reliability of these consumer-grade devices and developing robust algorithms to filter out artifacts and interpret the data effectively within the context of a patient’s overall health.

AI-Powered ECG Interpretation and Predictive Analytics
Artificial intelligence is transforming ECG interpretation, moving beyond simple pattern recognition to sophisticated predictive analytics. Machine learning models are being trained on vast datasets of ECGs to identify subtle indicators of cardiac disease that may not be apparent with traditional methods. These AI systems can predict the risk of future cardiac events, such as heart attacks or heart failure, with increasing accuracy. For instance, AI algorithms can analyze the complex interplay between different ECG parameters, including T-wave characteristics, to provide a more nuanced risk stratification. The ongoing research and development in this area promise to make ECGs even more powerful diagnostic tools, shifting the paradigm from reactive treatment to proactive prevention and personalized cardiac management. The ethical implications of AI in healthcare, including data privacy and algorithmic bias, are also critical areas of ongoing technological and societal discussion.
