The question of what causes meningitis is a critical one, touching upon infectious diseases and public health. While the human body is a remarkable system, it can fall victim to various pathogens that trigger inflammation of the meninges, the protective membranes surrounding the brain and spinal cord. Understanding the causative agents is the first step in prevention, diagnosis, and effective treatment of this potentially life-threatening condition. This exploration delves into the primary culprits behind meningitis, differentiating between the major categories of infectious agents and the specific organisms within them.
Bacterial Meningitis: A Rapid and Severe Threat
Bacterial meningitis stands out due to its swift onset and high severity, often progressing from initial symptoms to critical illness within hours. The pathogens responsible are diverse, but a few key players are responsible for the majority of cases. Prompt recognition of symptoms and immediate medical intervention, including antibiotic treatment, are paramount for survival and minimizing long-term complications.
Key Bacterial Pathogens
Several types of bacteria are commonly implicated in meningitis. The specific bacterium often depends on the age of the affected individual and their vaccination status.
Streptococcus pneumoniae (Pneumococcal Meningitis)
Streptococcus pneumoniae, also known as pneumococcus, is a leading cause of bacterial meningitis in adults and children worldwide. This gram-positive bacterium is a common resident of the nasopharynx (the upper part of the throat behind the nose) in many healthy individuals. However, under certain circumstances, it can breach the body’s defenses and enter the bloodstream, eventually reaching the meninges. Factors that increase the risk of pneumococcal meningitis include weakened immune systems (due to conditions like HIV, cancer, or organ transplantation), chronic illnesses (such as diabetes or lung disease), and lack of vaccination. The conjugate vaccine against Streptococcus pneumoniae has significantly reduced the incidence of pneumococcal meningitis, particularly in young children.
Neisseria meningitidis (Meningococcal Meningitis)
Neisseria meningitidis, or the meningococcus, is another significant cause of bacterial meningitis, particularly notorious for causing outbreaks in close-contact settings like college dormitories, military barracks, and refugee camps. This gram-negative bacterium is also a nasopharyngeal colonizer. Meningococcal meningitis can progress very rapidly and is often associated with a characteristic rash that does not fade when pressed (non-blanching petechiae or purpura), indicating a more severe form of the disease called meningococcemia. There are several serogroups of Neisseria meningitidis (A, B, C, W, and Y being the most common), and vaccines are available for many of these. However, the emergence of new serogroups or strains can pose ongoing challenges to public health efforts.
Haemophilus influenzae type b (Hib Meningitis)
Before the widespread introduction of the Hib vaccine, Haemophilus influenzae type b was a leading cause of bacterial meningitis in infants and young children. This small, pleomorphic gram-negative coccobacillus can cause severe invasive diseases beyond meningitis, including epiglottitis and pneumonia. The development and successful implementation of the Hib conjugate vaccine have dramatically reduced the incidence of Hib meningitis in countries with high vaccination rates, showcasing the immense impact of public health interventions. However, Hib meningitis can still occur in unvaccinated populations or in individuals with compromised immune systems.
Listeria monocytogenes (Listeriosis)
Listeria monocytogenes is a gram-positive bacterium that can cause meningitis, particularly in neonates, pregnant women, the elderly, and immunocompromised individuals. Unlike many other bacterial causes of meningitis, Listeria is found in the environment, particularly in soil, water, and animal feces. It is often contracted through contaminated food, such as unpasteurized dairy products, deli meats, and raw sprouts. Listeriosis can cause a range of symptoms, from mild flu-like illness to severe meningitis and septicemia. Pregnant women infected with Listeria can transmit the infection to their fetus, leading to miscarriage, stillbirth, or serious illness in the newborn.
Other Bacterial Causes
While the above are the most common culprits, other bacteria can also cause meningitis. These include:
- Group B Streptococcus (GBS): A common cause of meningitis in newborns, often acquired during birth from the mother.
- Gram-negative bacilli: Such as Escherichia coli (E. coli), Pseudomonas aeruginosa, and Klebsiella pneumoniae, which can cause meningitis, particularly in premature infants, individuals with shunts or catheters, or those with severe underlying illnesses.
- Tuberculosis (TB) bacilli (Mycobacterium tuberculosis): Can cause a chronic, slow-developing form of meningitis known as tuberculous meningitis, which is particularly prevalent in regions with a high burden of TB.
Viral Meningitis: The Most Common, Often Milder Form
Viral meningitis is significantly more common than bacterial meningitis and is generally less severe. While still capable of causing considerable discomfort and illness, viral meningitis often resolves on its own without specific antiviral treatment. The causative viruses are numerous, and their transmission routes vary.
Common Viral Pathogens
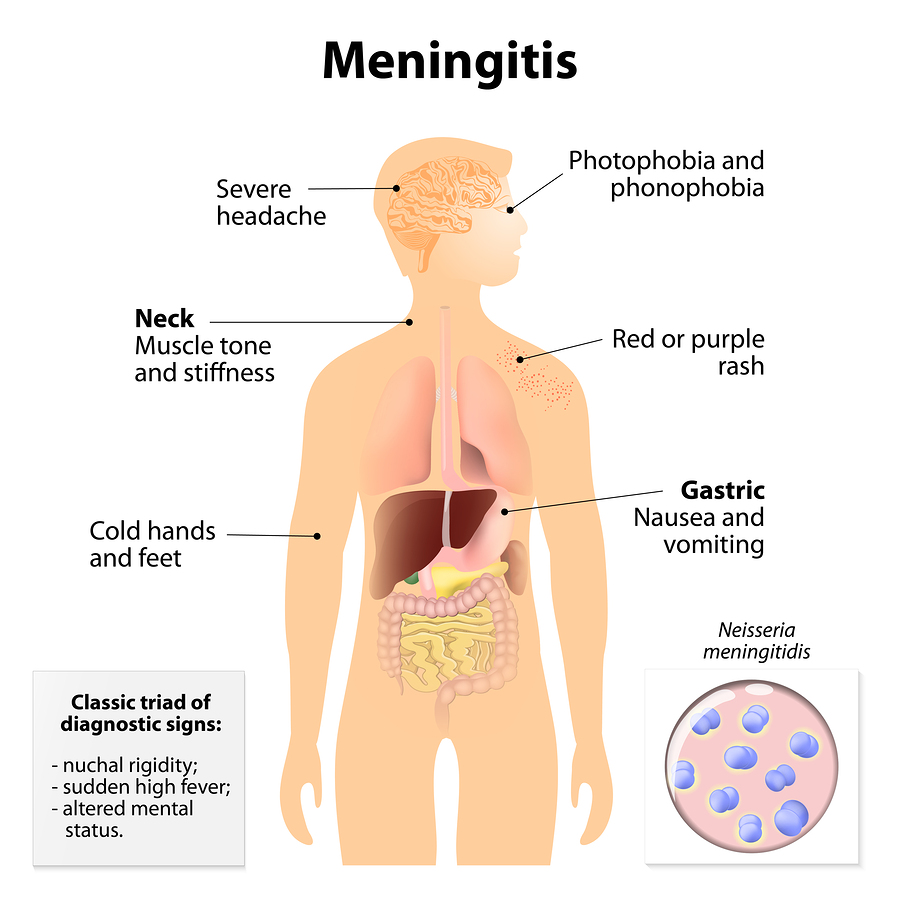
The vast majority of viral meningitis cases are caused by a group of viruses known as enteroviruses.
Enteroviruses
Enteroviruses are a large group of RNA viruses that are responsible for a wide spectrum of illnesses, including common colds, hand, foot, and mouth disease, and, importantly, viral meningitis. These viruses are highly contagious and are often spread through the fecal-oral route, meaning they can be transmitted through contaminated food or water, or by direct contact with infected individuals. Symptoms of enteroviral meningitis can include fever, headache, stiff neck, sensitivity to light, and sometimes a rash. While most cases are mild, some individuals, particularly infants, can develop more severe complications.
Other Viral Causes
Besides enteroviruses, several other viruses can trigger meningitis:
- Herpes Simplex Viruses (HSV): HSV-1 and HSV-2, the viruses responsible for cold sores and genital herpes, can also cause meningitis, particularly a severe form known as herpes simplex encephalitis when the brain tissue itself is infected.
- Mumps Virus: Before widespread mumps vaccination, mumps was a significant cause of viral meningitis. While still circulating, its incidence has been greatly reduced by the MMR (measles, mumps, rubella) vaccine.
- West Nile Virus (WNV): Transmitted through the bite of infected mosquitoes, WNV can cause a range of neurological illnesses, including meningitis and encephalitis.
- Arboviruses (e.g., Eastern Equine Encephalitis, Western Equine Encephalitis): These viruses, also transmitted by mosquitoes, can cause severe forms of meningitis and encephalitis, particularly in specific geographic regions.
- Varicella-Zoster Virus (VZV): The virus responsible for chickenpox and shingles can, in rare cases, cause meningitis.
- Human Immunodeficiency Virus (HIV): While HIV primarily targets the immune system, it can also directly or indirectly lead to meningitis.
Fungal Meningitis: A Rare but Serious Concern, Especially in Immunocompromised Individuals
Fungal meningitis is considerably rarer than bacterial or viral meningitis but can be particularly devastating, especially for individuals with weakened immune systems. The fungi responsible are typically found in the environment, and infection usually occurs through inhalation or, in some cases, through contaminated medical procedures.
Key Fungal Pathogens
The most common causes of fungal meningitis are yeasts and molds that can thrive in various environmental settings.
Cryptococcus neoformans
Cryptococcus neoformans is a yeast that is a leading cause of fungal meningitis, particularly in individuals with compromised immune systems, such as those with advanced HIV/AIDS. This yeast is commonly found in soil contaminated with bird droppings. Infection typically occurs through inhalation of the fungal spores. Once in the lungs, the fungus can enter the bloodstream and spread to the central nervous system. Cryptococcal meningitis can be slow to develop and is associated with significant morbidity and mortality if not treated promptly and effectively with antifungal medications.
Candida species
Various species of Candida, a type of yeast normally found on the skin and mucous membranes, can cause fungal meningitis. While Candida infections are more common in hospital settings, particularly in critically ill patients or those with indwelling medical devices, invasive candidiasis including meningitis can occur in immunocompromised individuals or following surgery.
Other Fungal Causes
Less commonly, other fungi such as Histoplasma capsulatum, Coccidioides immitis, and Blastomyces dermatitidis can cause meningitis, often in specific geographic regions or in individuals with particular exposure histories. These fungi are typically found in soil or endemic areas and can be inhaled.
Other Causes of Meningitis
While infectious agents are the primary drivers of meningitis, other factors can lead to inflammation of the meninges, though these are less common.
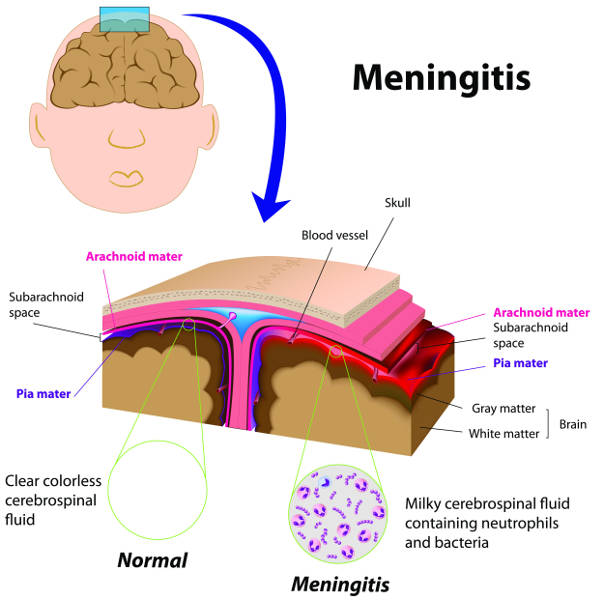
Non-Infectious Causes
- Autoimmune Diseases: Certain autoimmune conditions, where the body’s immune system mistakenly attacks its own tissues, can lead to inflammation of the meninges. Examples include lupus (systemic lupus erythematosus) and sarcoidosis.
- Cancer: In some cases, cancer cells can spread to the meninges (leptomeningeal carcinomatosis), causing inflammation and neurological symptoms. This is more common with certain types of cancer, such as breast, lung, and melanoma.
- Drug Reactions: A small number of medications can trigger an allergic reaction that causes meningitis.
- Trauma or Surgery: Head injuries or neurosurgical procedures can sometimes lead to inflammation of the meninges, either due to direct injury or as a complication of infection following the procedure.
Understanding the diverse etiologies of meningitis is crucial for guiding diagnostic approaches and selecting appropriate treatment strategies. Early recognition of symptoms and prompt medical attention are critical for all forms of meningitis, but especially for the bacterial and fungal varieties, where timely intervention can significantly improve outcomes and prevent devastating long-term consequences.
