The discomfort of thrush in the mouth can manifest in various ways, affecting taste, sensation, and overall oral comfort. Understanding these sensations is the first step toward recognizing the condition and seeking appropriate relief. This article delves into the typical feelings and experiences associated with oral thrush, offering insights for those who suspect they may be affected.
The Sensations of Oral Thrush: A Comprehensive Overview
Oral thrush, medically known as oral candidiasis, is a common fungal infection caused by an overgrowth of Candida albicans, a type of yeast that naturally resides in the mouth. While normally harmless, an imbalance in the oral environment can lead to its proliferation, resulting in a range of unpleasant sensations. These sensations can vary in intensity and presentation, impacting daily activities like eating, drinking, and speaking.
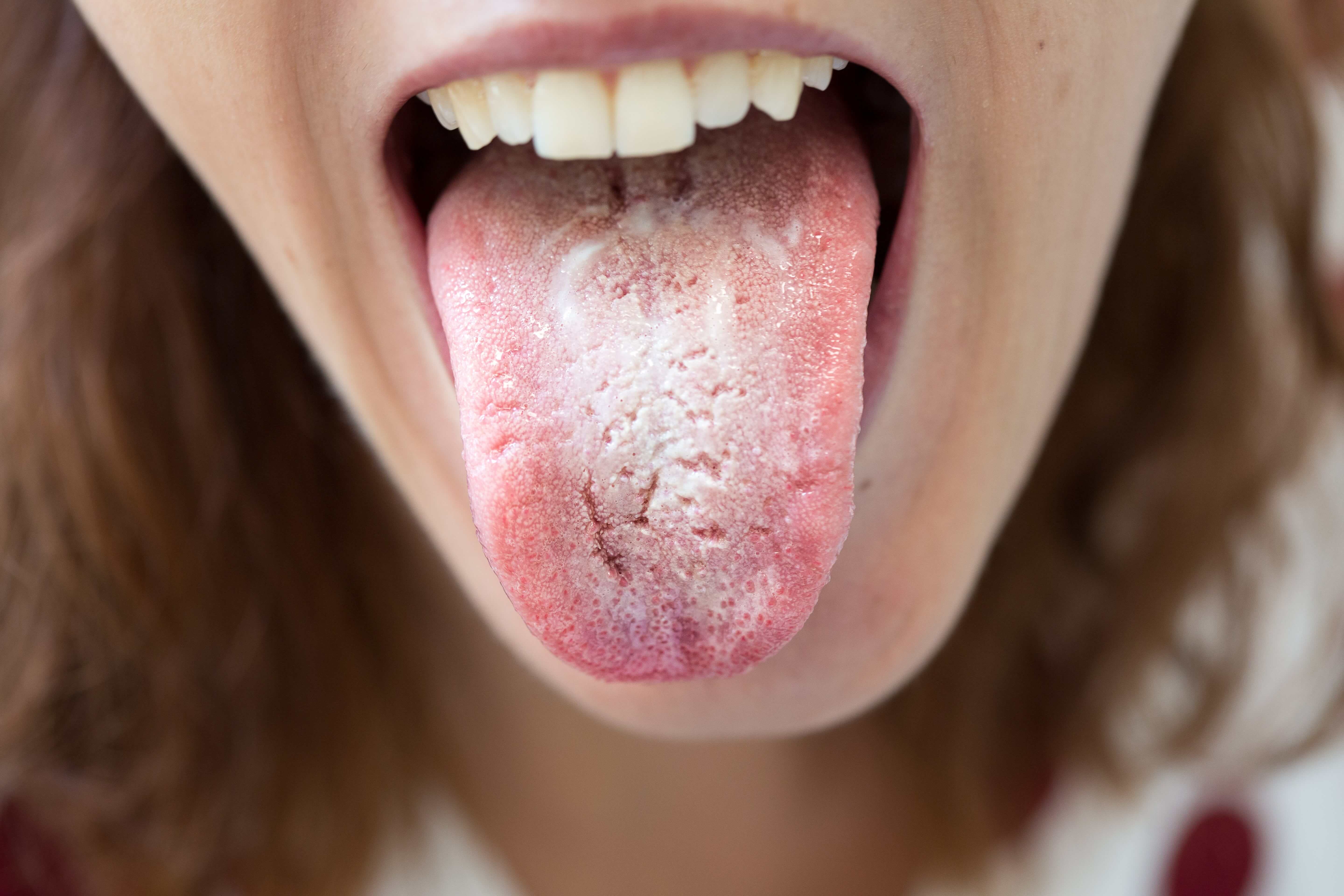
Burning and Soreness: The Primary Discomfort
Perhaps the most frequently reported symptom of oral thrush is a burning sensation in the mouth. This can be a persistent, low-grade ache or a more intense, stinging discomfort. The tongue, cheeks, palate, and gums can all feel inflamed and irritated. This burning sensation is often exacerbated by certain foods or drinks, particularly those that are spicy, acidic, or very hot, which can further aggravate the already sensitive oral tissues.
Alongside the burning, soreness is another prominent feeling. The mouth might feel raw and tender, making even the gentlest touch of a toothbrush uncomfortable. This soreness can lead to a general reluctance to eat, as the act of chewing and swallowing becomes a painful experience. The inflammation associated with thrush can cause the oral tissues to appear red and inflamed, contributing to the overall feeling of soreness and discomfort.
Changes in Taste and Texture: A Palate Disrupted
Many individuals experiencing oral thrush report a noticeable alteration in their sense of taste. Food may start to taste bland, metallic, or even unpleasant. This distortion of taste can significantly impact appetite and enjoyment of meals, leading to nutritional concerns if left unaddressed. The fungal overgrowth can interfere with the taste buds’ ability to properly detect flavors.
Beyond taste, the texture of the tongue and other oral surfaces can also feel altered. A common description is a cottony or fuzzy feeling in the mouth. This is often due to the creamy white patches that characterize thrush, which can coat the tongue and the inside of the cheeks. These patches can create a physical barrier, contributing to the feeling of a dry or coated tongue, even when adequate fluids are consumed. Some individuals may also experience a feeling of stickiness or a slimy sensation in their mouth.
Difficulty Swallowing and Speaking: Impact on Function
In more severe cases, oral thrush can extend to the throat, causing discomfort and difficulty when swallowing. This odynophagia, or painful swallowing, can range from a mild tickle or irritation to significant pain that makes eating and drinking a challenging ordeal. The inflammation can affect the pharynx, making the passage of food and liquids feel rough or obstructed.
The discomfort and physical presence of the fungal patches can also impact speech. Some individuals report a feeling of thickness in their mouth or a slight impediment to their articulation. While not as common as taste or pain alterations, this functional impact can add to the overall distress caused by oral thrush. The discomfort can lead to a tendency to speak with less volume or to avoid talking unnecessarily.
Itching and Irritation: Persistent Annoyances
Beyond the more acute sensations of burning and soreness, oral thrush can also be accompanied by a persistent feeling of itching and general irritation within the mouth. This itching can be subtle or more pronounced, leading to an urge to scratch or rub the affected areas. While scratching might offer temporary relief, it can also further irritate the delicate oral tissues, potentially worsening the condition.
This ongoing irritation can make it difficult to focus on tasks, disrupt sleep, and generally detract from one’s quality of life. The constant awareness of an uncomfortable sensation within the mouth can be a significant psychological burden, adding to the physical discomfort.
Other Potential Sensations and Signs
While the above are the most common experiences, other sensations can also be associated with oral thrush:
- Dry Mouth (Xerostomia): Although the patches themselves can create a feeling of coated dryness, some individuals also experience a genuine reduction in saliva production, contributing to a dry mouth sensation.
- Cracking at the Corners of the Mouth: In some cases, oral thrush can lead to angular cheilitis, which presents as cracking, redness, and soreness at the corners of the mouth. This can feel like painful fissures that make opening the mouth wide or eating difficult.
- White Patches or Plaques: The most visible sign of oral thrush is the presence of creamy white, cottage cheese-like patches on the tongue, inner cheeks, roof of the mouth, gums, or tonsils. While not a “feeling” in itself, the presence of these patches is often directly linked to the sensations experienced. If these patches are scraped off, they may reveal red, inflamed, and sometimes bleeding tissue underneath, contributing to the soreness and burning.
It is important to note that the intensity and combination of these sensations can vary significantly from person to person. Factors such as the extent of the infection, the individual’s immune system status, and the presence of any underlying medical conditions can all influence how oral thrush feels.
Identifying Thrush: When to Seek Professional Advice
Recognizing the distinctive sensations associated with oral thrush is crucial for timely diagnosis and effective treatment. While occasional mild oral discomfort can be attributed to various factors, a persistent pattern of burning, soreness, altered taste, or the characteristic cottony feeling warrants attention from a healthcare professional.

Distinctive Symptoms and Visual Cues
The presence of the hallmark creamy white patches is a strong indicator of oral thrush. These patches are typically found on the tongue, inner cheeks, palate, and throat. When scraped, these patches may leave behind red, inflamed areas that can bleed easily. This visual evidence, combined with the subjective sensations described above, forms the basis for a presumptive diagnosis.
The burning and soreness often accompany these visual cues, creating a palpable discomfort. The feeling of a coated or fuzzy tongue, coupled with a metallic or unpleasant taste, further reinforces the suspicion of an infection. It is the combination of these sensory experiences and visual manifestations that prompts many individuals to seek medical evaluation.
Underlying Causes and Risk Factors
Oral thrush can be triggered or exacerbated by several factors that disrupt the natural balance of microorganisms in the mouth. Understanding these underlying causes can help in identifying individuals at higher risk and in preventing recurrence.
- Weakened Immune System: Conditions that compromise the immune system, such as HIV/AIDS, cancer, or treatments like chemotherapy and radiation therapy, make individuals more susceptible to Candida overgrowth.
- Diabetes: High blood sugar levels can provide a fertile ground for yeast to thrive. Individuals with poorly controlled diabetes are at increased risk.
- Antibiotic Use: Antibiotics kill not only harmful bacteria but also beneficial bacteria in the mouth that help keep yeast in check. This imbalance can lead to a yeast overgrowth.
- Steroid Inhalers: The use of corticosteroid inhalers for conditions like asthma can lead to a buildup of the medication in the mouth, creating an environment conducive to yeast growth. Rinsing the mouth after using such inhalers is often recommended.
- Denture Use: Poorly fitting or unclean dentures can create areas where yeast can accumulate and multiply.
- Dry Mouth (Xerostomia): Saliva plays a crucial role in keeping the mouth clean and moist, and it helps to control yeast growth. Conditions or medications that cause dry mouth can increase the risk of thrush.
- Pregnancy: Hormonal changes during pregnancy can sometimes lead to an increased susceptibility to fungal infections, including oral thrush.
Recognizing these risk factors in oneself or in others can be an important step in proactive health management and in understanding why oral thrush might develop.
When to Consult a Doctor or Dentist
If you experience any of the characteristic symptoms of oral thrush, especially if they are persistent or severe, it is essential to consult a healthcare professional. This includes your primary care physician or a dentist. They can accurately diagnose the condition, rule out other potential oral health issues, and prescribe the most appropriate treatment.
Early diagnosis and treatment are key to alleviating discomfort, preventing the infection from spreading, and addressing any underlying contributing factors. Self-treating oral thrush without a proper diagnosis can be ineffective and may delay the appropriate care needed to resolve the infection.
Managing and Treating Oral Thrush: From Home Remedies to Medical Interventions
Once oral thrush is diagnosed, a range of treatment options are available, varying from simple home care strategies to prescribed antifungal medications. The goal of treatment is to eliminate the excess yeast, restore the balance of microorganisms in the mouth, and alleviate the associated symptoms.
Antifungal Medications: The Cornerstone of Treatment
The primary medical treatment for oral thrush involves antifungal medications. These are available in various forms, including:
- Topical Antifungals: These are usually the first line of treatment for mild to moderate cases. They are applied directly to the affected areas in the mouth. Common forms include:
- Nystatin: This is often prescribed as a liquid suspension that is swished around the mouth and then swallowed, or as lozenges.
- Clotrimazole: This is typically prescribed as a lozenge or troche that is dissolved in the mouth.
- Miconazole: Available as an oral gel or in a buccal tablet form.
- Systemic Antifungals: For more severe or persistent cases, or if the infection has spread to the esophagus, oral antifungal medications that are taken by mouth are prescribed.
- Fluconazole: This is the most commonly prescribed oral antifungal for thrush. It is a pill that is taken for a specific duration.
- Itraconazole: Another oral antifungal that may be used in certain situations.
It is crucial to complete the entire course of antifungal medication as prescribed by your healthcare provider, even if your symptoms improve. Stopping treatment prematurely can lead to the infection returning.
Home Care and Supportive Measures: Enhancing Recovery
In conjunction with medical treatment, several home care practices can help manage symptoms and support recovery:
- Maintain Good Oral Hygiene: Brush your teeth gently twice a day with a soft-bristled toothbrush and fluoride toothpaste. Avoid harsh brushing that can irritate the inflamed tissues.
- Rinse Your Mouth: After using steroid inhalers, rinse your mouth thoroughly with water to remove any residual medication. Some healthcare providers may recommend rinsing with a saltwater solution or a baking soda and water solution to help maintain an alkaline environment in the mouth, which can be less favorable for yeast.
- Stay Hydrated: Drink plenty of water to keep your mouth moist. Sip water or sugar-free beverages throughout the day.
- Dietary Considerations: While not a cure, some individuals find relief by avoiding foods and drinks that can irritate their mouth, such as very hot, spicy, acidic, or sugary items. Consider consuming bland foods and soft textures.
- Clean Dentures and Oral Appliances: If you wear dentures, remove them at night and clean them thoroughly each day according to your dentist’s instructions. Ensure they fit properly, as ill-fitting dentures can contribute to thrush.

Addressing Underlying Causes: Long-Term Prevention
Effective management of oral thrush also involves addressing any underlying conditions that may have contributed to its development. This might include:
- Managing Diabetes: Working with a healthcare provider to achieve better blood sugar control.
- Reviewing Medications: Discussing with your doctor if any medications you are taking might be contributing to thrush and exploring potential alternatives or adjustments.
- Boosting Immune System: For individuals with compromised immune systems, managing the underlying condition is paramount.
By understanding the various ways oral thrush can feel, recognizing its signs, and actively participating in treatment and preventive measures, individuals can effectively manage this common fungal infection and regain comfort in their oral health.
