The arrival of cooler weather often heralds a familiar trio of seasonal discomforts: the common cold, the influenza virus (flu), and increasingly, concerns about respiratory health in the context of technological advancements. While the terms “cold” and “flu” are frequently used interchangeably in everyday conversation, understanding their fundamental differences is crucial for effective self-care, informed healthcare decisions, and even for appreciating the context within which we discuss public health. This article delves into the distinct characteristics of these two prevalent respiratory illnesses, exploring their causative agents, symptom presentation, severity, and implications, all within the framework of how we perceive and manage health in a technologically driven world.

The Microbial Architects: Viruses as the Primary Culprits
At the heart of both colds and the flu lies their viral origin. However, the specific families of viruses responsible and their modes of transmission play a significant role in differentiating the two. Understanding these microbial architects provides a foundational insight into the distinct pathological processes they instigate.
Cold Viruses: The Rhinovirus Dominance
The vast majority of common colds are caused by rhinoviruses, belonging to the Picornaviridae family. There are over 100 distinct serotypes of rhinoviruses, explaining why individuals can experience multiple colds throughout their lives. Other viruses, such as adenoviruses, coronaviruses (not the SARS-CoV-2 strain responsible for COVID-19, but others that cause milder symptoms), and parainfluenza viruses, can also contribute to cold symptoms. These viruses primarily infect the upper respiratory tract – the nose and throat. Transmission typically occurs through airborne droplets produced when an infected person coughs, sneezes, or talks, or by direct contact with contaminated surfaces. The relatively smaller size of these viral particles and their limited capacity for rapid replication within the host contribute to the generally milder and more localized nature of cold symptoms. The immune system’s response, while effective, is often geared towards neutralizing these specific, less virulent invaders, leading to a more manageable host response.
Influenza Viruses: The Orthomyxoviridae Threat
Influenza, or the flu, is caused by influenza viruses, which belong to the Orthomyxoviridae family. There are three main types of influenza viruses that infect humans: types A, B, and C. Influenza A and B viruses are responsible for seasonal epidemics, while influenza C viruses typically cause milder respiratory illness. Influenza A viruses are further classified into subtypes based on two surface proteins: hemagglutinin (H) and neuraminidase (N). The constant evolution of these surface proteins, particularly through antigenic drift (minor genetic changes) and antigenic shift (major genetic reassortment), necessitates the annual reformulation of influenza vaccines. Unlike cold viruses that primarily target the upper respiratory tract, influenza viruses can infect both the upper and lower respiratory tracts, including the lungs. This broader infectivity, coupled with the virus’s potent replication capabilities, contributes to the more severe and systemic nature of flu symptoms. The immune system’s response to influenza is often more robust and widespread, leading to the characteristic inflammatory cascade that defines flu illness.
Symptom Spectrum: A Tale of Two Illnesses
While both colds and the flu manifest with respiratory symptoms, the onset, severity, and specific characteristics of these symptoms offer a clear distinction between the two. Recognizing these differences is paramount for appropriate self-management and seeking timely medical attention when necessary.
The Gradual Onset of a Cold
The onset of common cold symptoms is typically gradual, often developing over a day or two. The hallmark signs of a cold usually begin with a sore throat, which may feel scratchy or irritated. This is frequently followed by a runny nose, which may start with clear mucus and then thicken and turn yellow or green as the illness progresses. Nasal congestion, sneezing, and a mild cough are also common. Adults with colds generally experience milder symptoms, and while fatigue may be present, it is usually not debilitating. Fever is less common in adults with colds, and when it occurs, it is typically low-grade. Children, however, are more prone to developing a fever with a cold. The overall feeling of malaise is usually less severe than with the flu, allowing many individuals to continue with their daily activities, albeit with some discomfort. The localized inflammation in the nasal passages and throat, driven by the rhinoviruses, dictates the primary symptom cluster.
The Abrupt and Intense Nature of the Flu
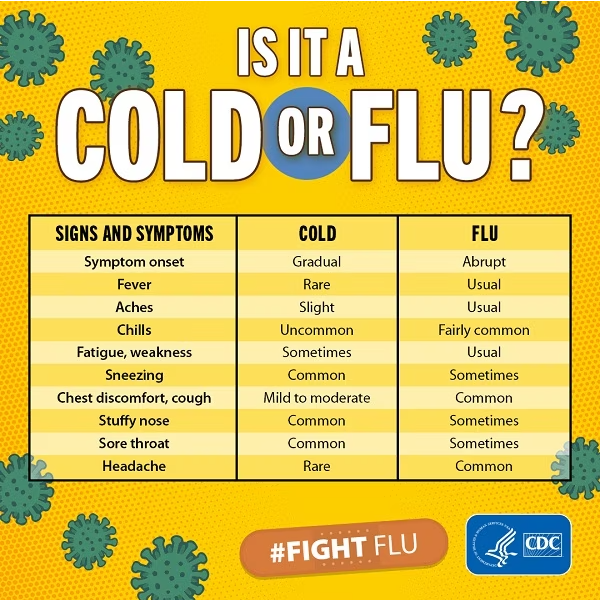
In stark contrast to the cold’s gentle arrival, influenza symptoms tend to manifest abruptly and intensely. Within a few hours to a day of infection, individuals often experience a sudden onset of fever, which can be high (100.4°F or higher), accompanied by chills. Body aches and muscle pain (myalgia) are a prominent feature of the flu, often described as feeling like being hit by a truck. Headaches are common and can be severe. A dry, hacking cough is also characteristic of the flu, and it can persist for weeks. Fatigue and weakness can be profound, often rendering individuals unable to perform their usual daily tasks and necessitating significant rest. While a sore throat and runny nose can occur with the flu, they are often less prominent than the systemic symptoms like fever, aches, and fatigue. The more aggressive replication and broader impact of influenza viruses on the body’s systems explain the rapid onset and severity of flu symptoms.
Severity and Complications: The Flu’s Potentially Serious Footprint
While both colds and flu can cause discomfort, the potential for severe illness and complications significantly differentiates the two. The flu, particularly in certain populations, carries a greater risk of serious health consequences that warrant prompt medical intervention.
The Generally Benign Course of a Cold
For most healthy individuals, the common cold is a self-limiting illness that resolves within a week to ten days. The primary concern with a cold is typically the discomfort it causes and the potential for it to disrupt daily life temporarily. However, certain complications can arise, particularly in individuals with pre-existing respiratory conditions or weakened immune systems. These can include sinus infections (sinusitis), ear infections (otitis media), and exacerbations of asthma or chronic obstructive pulmonary disease (COPD). These secondary infections occur when the initial viral infection compromises the body’s defenses, allowing bacteria to gain a foothold. While uncomfortable, these complications are generally manageable with appropriate medical care and do not typically pose a life-threatening risk for otherwise healthy individuals. The localized nature of the viral infection in the upper respiratory tract limits the systemic impact and the likelihood of widespread organ involvement.
The Flu’s Capacity for Serious Illness
Influenza can lead to significant and sometimes life-threatening complications. The most common complication of the flu is pneumonia, which can be caused by the influenza virus itself (viral pneumonia) or by a secondary bacterial infection (bacterial pneumonia) that takes advantage of the weakened respiratory system. Other serious complications include bronchitis, sinus infections, and ear infections. For individuals with chronic health conditions such as heart disease, lung disease (including asthma), diabetes, or weakened immune systems (due to conditions like HIV/AIDS or cancer treatment), the flu can lead to a dangerous worsening of their underlying illness. In severe cases, influenza can cause inflammation of the heart (myocarditis), brain (encephalitis), or muscles (myositis), and can lead to multi-organ failure. The elderly, young children, pregnant women, and individuals with certain medical conditions are at higher risk for developing severe flu-related complications. The systemic nature of influenza infection and its propensity to attack the lower respiratory tract makes it a considerably more formidable threat than the common cold.
Prevention and Management: A Proactive Approach to Respiratory Health
Understanding the differences between colds and the flu is not just about academic knowledge; it informs our strategies for prevention and management, enabling us to make informed decisions about our health and well-being. This is particularly relevant in an era where technological advancements offer new tools for health monitoring and disease surveillance.
Cold Prevention and Symptom Relief
Preventing the common cold largely revolves around good hygiene practices. Frequent handwashing with soap and water for at least 20 seconds is paramount to removing viruses from surfaces. Avoiding close contact with sick individuals, not touching your eyes, nose, and mouth with unwashed hands, and disinfecting frequently touched surfaces can also significantly reduce the risk of transmission. When you do come down with a cold, the focus is on symptom relief. Rest, adequate fluid intake (water, broth, herbal teas), and over-the-counter medications such as decongestants, pain relievers (acetaminophen or ibuprofen), and cough suppressants can help manage discomfort. It’s important to note that antibiotics are ineffective against viruses and should not be used for treating colds. Home remedies like gargling with salt water for a sore throat or using a humidifier to ease congestion can also provide relief. The gradual onset and less severe nature of colds allow for a more self-directed management approach.

Flu Prevention: The Power of Vaccination and Vigilance
The most effective way to prevent influenza and its potentially serious complications is through annual vaccination. The influenza vaccine is recommended for most people aged six months and older. While the vaccine is not 100% effective, it significantly reduces the risk of contracting the flu, and if infection does occur, it can lessen the severity of the illness and the likelihood of complications. In addition to vaccination, good hygiene practices, similar to those for preventing colds, are crucial. This includes frequent handwashing, avoiding close contact with sick individuals, and covering coughs and sneezes. Antiviral medications can be prescribed by a doctor to treat the flu, especially for individuals at high risk of complications. These medications are most effective when started within 48 hours of symptom onset and can help reduce the duration and severity of illness. Recognizing flu symptoms early and seeking medical advice is vital, especially for vulnerable populations. The proactive approach to flu prevention, particularly through vaccination, underscores its greater public health significance compared to the common cold.
In conclusion, while both the common cold and influenza are respiratory illnesses caused by viruses, they are distinct entities with differing etiologies, symptom profiles, and potential for severity. Recognizing these differences empowers individuals to make informed decisions regarding prevention, seeking appropriate medical care when necessary, and ultimately, safeguarding their health in an ever-evolving world where understanding our biological vulnerabilities remains as critical as embracing technological progress.
